Topol E, et al. “An international randomized trial comparing four thrombolytic strategies for acute myocardial infarction”. The New England Journal of Medicine. 1993. 329(10):673-682.
Cohen M, et al. “A Comparison of Low-Molecular-Weight Heparin with Unfractionated Heparin for Unstable Coronary Artery Disease”. The New England Journal of Medicine. 1997. 337(7):447-452.
Hochman J.S., et al. “Coronary Intervention for Persistent Occlusion after Myocardial Infarction”. The New England Journal of Medicine. 2006. 355(23):2395-2407.
McFalls EO, et al. “Coronary-artery revascularization before elective major vascular surgery”. The New England Journal of Medicine. 2004. 351(27):2795-2804.
Holzer M, et al. “Mild Therapeutic Hypothermia to Improve the Neurologic Outcome After Cardiac Arrest”. The New England Journal of Medicine. 2002. 346(8):549-556.
Marso SP, et al. “Liraglutide and cardiovascular outcomes in type 2 diabetes”. The New England Journal of Medicine. 2016. 375(4):311-322.
ARISE Trial. “Goal-directed resuscitation for patients with early septic shock”. The New England Journal of Medicine. 2014. 371(16):1496-1506.
Lamontagne, F, et al. “Intravenous Vitamin C in Adults with Sepsis in the Intensive Care Unit”. New England Journal of Medicine. 2022. 386(25):2387-2398.
Fujii T, et al. “Effect of vitamin C, hydrocortisone, and thiamine vs hydrocortisone alone on time alive and free of vasopressor support among patients with septic shock: The VITAMINS randomized clinical trial”. JAMA. 2020. 323(5):423-431.
The implementation of an analgesia-based sedation protocol reduced deep sedation and proved to be safe and feasible in patients on mechanical ventilation.
Non-steroidal anti-inflammatory drugs in treatment of postoperative pain after cardiac surgery.
PROCESS trial: Protocol-based therapy for septic shock
Psychiatric outcomes of patients with severe agitation following administration of prehospital ketamine.
Gibson CM, et al. “Prevention of bleeding in patients with AF undergoing PCI”. The New England Journal of Medicine. 2016. epub 2016-11-14:1-12.
Moss AJ, et al. “Prophylactic Implantation of a Defibrillator in Patients with Myocardial Infarction and Reduced Ejection Fraction”. The New England Journal of Medicine. 2002. 346(12):877-883.
Swedberg K, et al. “Treatment of anemia with darbepoetin alfa in systolic heart failure”. The New England Journal of Medicine. 2013. 368(13):1210-9.
Manson JE, et al. “Vitamin D supplements and prevention of cancer and cardiovascular disease”. The New England Journal of Medicine. 2019. 380(1):33-44.
Pitt B, et al. “Eplerenone, a selective aldosterone blocker, in patients with left ventricular dysfunction after myocardial infarction”. The New England Journal of Medicine. 2003. 348(14):1309-21.
Bonaca MP, et al. “Long-term use of ticagrelor in patients with prior myocardial infarction”. The New England Journal of Medicine. 2015. 372(19):1791-1800.
Rapid tranquillisation for agitated patients in emergency psychiatric rooms: a randomised trial of midazolam versus haloperidol plus promethazine.
Echt DS, et al. “Mortality and morbidity in patients receiving encainide, flecainide, or placebo”. The New England Journal of Medicine. 1991. 324(12):781-788.
Acetylcysteine for Prevention of Renal Outcomes in Patients Undergoing Angiography”. Circulation. 2011. 124:1250-1259
Bandstein N, et al. “Undetectable high-sensitivity cardiac troponin T level in the emergency department and risk of myocardial infarction”. Journal of the American College of Cardiology. 2014. 63(23):2569-2578.
Midazolam and propofol used alone or sequentially for long-term sedation in critically ill, mechanically ventilated patients: A prospective, randomized study.
Intermittent Versus Continuous Infusion Dosing of Intravenous Proton Pump Inhibitors
Dankiewicz J, et al. “Hypothermia versus Normothermia after Out-of-Hospital Cardiac Arrest”. The New England Journal of Medicine. 2021. 384(24):2283-2294.
Rapid tranquillisation in psychiatric emergency settings in India: pragmatic randomised controlled trial of intramuscular olanzapine versus intramuscular haloperidol plus promethazine.
Yusuf S, et al. “Effects of Clopidogrel in Addition to Aspirin in Patients with Acute Coronary Syndromes without ST-Segment Elevation”. The New England Journal of Medicine. 2001. 345(7):494-502.
Tardif J, et al. “Efficacy and safety of low-dose colchicine after myocardial infarction”. The New England Journal of Medicine. 2019. 381(26):2497-2505.
NINDS: TISSUE PLASMINOGEN ACTIVATOR FOR ACUTE ISCHEMIC STROKE
Efficacy of perioperative pregabalin in acute and chronic post-operative pain after off-pump coronary artery bypass surgery: A randomized, double-blind placebo controlled trial.
The use of midazolam versus propofol for short-term sedation following coronary artery bypass grafting.
Midazolam versus propofol for long-term sedation in the ICU: A randomized prospective comparison.
Yusuf S, et al. “Comparison of fondaparinux and enoxaparin in acute coronary syndromes”. The New England Journal of Medicine. 2006. 354(14):1464-1476.
Dose comparisons of clopidogrel and aspirin in acute coronary syndromes
Hoberman A, Paradise JL, Rockette HE, et al. Shortened Antimicrobial Treatment for Acute Otitis Media in Young Children. N Engl J Med. 2016
Annane D, et al. “Hydrocortisone plus Fludrocortisone for Adults with Septic Shock”. The New England Journal of Medicine. 2018. 378(9):809-818.
Comparison of patient-controlled epidural analgesia with patient-controlled intravenous analgesia using pethidine or fentanyl.
Comparison of intramuscular and epidural morphine for postoperative analgesia in the grossly obese.
GUSTO Trial, 1993
Undetectable high-sensitivity cardiac troponin T level in the emergency department and risk of myocardial infarction
GISSI-3 Group. “Effects of lisinopril and transdermal glyceryl trinitrate singly and together on 6-week mortality and ventricular function after acute myocardial infarction”. The Lancet. 1994. 343(8906):1115-22.
PEGASUS-TIMI 54. Long-Term Use of Ticagrelor in Patients with Prior Myocardial Infarction
Clopidogrel and aspirin versus aspirin alone for the prevention of atherothrombotic events
FRISC Investigators. “Invasive compared with non-invasive treatment in unstable coronary-artery disease: FRISC II prospective randomised multicentre study”.
CAPRICORN Trial Dargie HJ, et al. “Effect of carvedilol on outcome after myocardial infarction in patients with left-ventricular dysfunction: the CAPRICORN randomised trial”. The Lancet. 2001. 357(9266):1385-1390.
Cumulative epinephrine dose during cardiac arrest and neurologic outcome after extracorporeal cardiopulmonary resuscitation
CAST Trial. Mortality and morbidity in patients receiving Encainide, Flecainide, or Placebo
BICAR-ICU
Statins for STEMI in the Emergency Department
Introduction
- STEMI (ST-Elevation Myocardial Infarction) represents a critical emergency where timely intervention is crucial. Atorvastatin, a statin, has been investigated for its potential benefits when administered early during a STEMI.
- Early administration of atorvastatin may have pleiotropic effects beyond cholesterol lowering. Potential benefits include stabilization of atherosclerotic plaques, reduction of inflammation, and improved endothelial function.
- Guidelines recommend initiating high-intensity statin therapy as soon as possible in STEMI patients.
- This pharmacy pearl summarizes the pharmacology and evidence supporting the use of atorvastatin in this setting.
Pharmacology
| Atorvastatin | Rosuvastatin | |
| Dose | 80 mg orally once daily | 40 mg orally once daily |
| Administration | Oral | Oral |
| PK/PD | Onset: 3-5 days for LDL reduction; Peak effect: 2-4 weeks | Onset: 3-5 days for LDL reduction; Peak effect: 2-4 weeks |
| Adverse Effects | Myopathy, elevated liver enzymes, gastrointestinal symptoms | Myopathy, elevated liver enzymes, gastrointestinal symptoms |
| Drug Interactions and warnings | CYP3A4 inhibitors/inducers can affect levels; avoid in active liver disease | Minimal CYP interactions; avoid in active liver disease |
| Compatibility | Compatible with most cardiovascular drugs, monitor for interactions with CYP3A4 inhibitors | Compatible with most cardiovascular drugs, minimal interactions |
| Comments | High-intensity statin recommended post-STEMI to reduce recurrence risk | High-intensity statin alternative to atorvastatin |
Overview of Evidence
| Author, Year | Design/Sample Size | Intervention & Comparison | Outcome | |
| Schwartz, 2001 | Randomized Controlled Trial (n=3086) | Atorvastatin (80 mg/day) vs. placebo initiated 2496 hours after acute coronary syndrome | Atorvastatin reduced recurrent symptomatic ischemia requiring rehospitalization (6.2% vs 8.4%; RR, 0.74; P=0.02) | |
| Li, 2012 | Randomized Controlled Trial (n=161) | High-dose atorvastatin (80 mg) vs. placebo in patients with STEMI undergoing PCI | High-dose atorvastatin significantly reduced the incidence of contrast-induced nephropathy (2.6% vs 15.7%; P=0.01) | |
| Liu, 2013 | Randomized Controlled Trial (n=102) | Loading dose of atorvastatin (80 mg) before PCI vs. no loading dose | Loading dose of atorvastatin reduced high-sensitivity C-reactive protein, B-type natriuretic peptide, and matrix metalloproteinase type 9, indicating reduced inflammation and improved cardiac function (P<0.05) | |
| Xu, 2016 | Randomized Controlled Trial (n=120) | Intensive atorvastatin (40 mg) vs. standard atorvastatin (20 mg) in STEMI patients undergoing PCI | Intensive atorvastatin significantly reduced serum endothelin-1 levels and ADP-induced platelet clot strength, improving endothelial function and platelet inhibition (P<0.05) | |
| Kim, 2015 | Randomized Controlled Trial (n=67) | High-dose atorvastatin (80 mg) before PCI vs. low-dose atorvastatin (10 mg) | No significant reduction in myocardial damage; however, high-dose pretreatment is generally considered safe and well-tolerated | |
| Gavazzoni, 2017 | Randomized Controlled Trial (n=52) | High-dose atorvastatin (80 mg) vs. moderate dose (20 mg) in STEMI patients | High-dose atorvastatin showed significant improvement in endothelial function (RH-PAT index 1.96±0.16 vs 1.72±0.19; P=0.002) and reduced levels of high-sensitivity CRP and IL6 (P<0.05) | |
| Liu, 2013 | Randomized Controlled Trial (n=102) | Loading dose of atorvastatin (80 mg) before PCI vs. no loading dose | Loading dose of atorvastatin significantly lowered inflammatory markers and improved left ventricular ejection fraction compared to no loading dose (P<0.05) | |
| Adel, 2022 | Randomized Controlled Trial (n=99) | High-dose rosuvastatin (40 mg) vs. high-dose atorvastatin (80 mg) before PCI in STEMI patients | Atorvastatin group had lower CTFC and better TIMI flow grade compared to control, and both statins improved microvascular myocardial perfusion (P<0.01) | |
| Chen, 2022 | Randomized Controlled Trial (n=98) | Enhanced-dose atorvastatin (40 mg before PCI, 40 mg/day post-PCI, 20 mg/day after 1 week) vs. standarddose atorvastatin (20 mg/day) | Enhanced-dose atorvastatin improved cardiac output, LVEF, TIMI blood flow classification, and reduced incidence of major adverse cardiac events (P<0.05) | |
Conclusions
- Efficacy: High-intensity atorvastatin (80 mg) initiated early in the ED for STEMI patients reduces the risk of subsequent cardiovascular events and mortality.
- Safety: Generally well-tolerated with a similar side effect profile to other statins, though monitoring for myopathy and liver enzyme elevations is necessary.
- Recommendation: Incorporating early administration of atorvastatin 80 mg for STEMI patients in the ED aligns with current guidelines and improves patient outcomes.
References
- Micromedex [Electronic version].Greenwood Village, CO: Truven Health Analytics. Retrieved July 1 2024, from http://www.micromedexsolutions.com/
- Schwartz GG, Olsson AG, Ezekowitz MD, et al. Effects of atorvastatin on early recurrent ischemic events in acute coronary syndromes: the MIRACL study: a randomized controlled trial. JAMA. 2001;285(13):1711-1718.
- Liu H, Yang Y, Yang SL, et al. Administration of a loading dose of atorvastatin before emergency PCI reduces myocardial damage in patients with STEMI. Clin Ther. 2013;35(1):22-30.
- Li W, Fu X, Wang Y, et al. Beneficial effects of high-dose atorvastatin pretreatment on microvascular obstruction and left ventricular function in STEMI patients undergoing primary PCI. Cardiology. 2012;123(4):212-220.
- Kim EK, Hahn J, Song Y, et al. Effects of high-dose atorvastatin pretreatment on microvascular obstruction in STEMI patients undergoing primary PCI. J Korean Med Sci. 2015;30(4):435-441.
- Xu X, Liu Y, Li K, et al. Intensive atorvastatin improves endothelial function and reduces inflammation in STEMI patients undergoing primary PCI. Int J Cardiol. 2016;220:616-621.
- Gavazzoni M, Lombardi CM, Vizzardi E, et al. Role of early high-dose atorvastatin loading in STsegment elevation myocardial infarction: real-life experience. J Cardiovasc Med (Hagerstown). 2017;18(6):406-411.
- Adel EM, Elberry A, Abdel Aziz A, Ibrahim MA, Abdelaal FA. Comparison of the treatment efficacy of rosuvastatin versus atorvastatin in preventing microvascular obstruction in patients undergoing primary PCI for STEMI. J Clin Med. 2022;11(17):5142.
- Chen Y, Zhang J, Huo Y, et al. Effects of atorvastatin on coronary microvascular function in STEMI patients undergoing primary PCI: a randomized controlled trial. J Am Coll Cardiol. 2022;79(9):901911.
Tranexamic Acid in Trauma by Jordan Spurling
Introduction
- Trauma is the leading cause of death in individuals up to 45 years old and the fourth leading cause of death overall for all ages.1
- Uncontrolled hemorrhage is the leading cause of early mortality in major trauma.2
- Trauma-associated hemorrhagic death occurs as an effect of uncontrolled bleeding and trauma-induced coagulopathy.3
- Tranexamic acid is an antifibrinolytic medication that works by forming a reversible complex that displaces plasminogen from fibrin resulting in inhibition of fibrinolysis.4
- Tranexamic acid is readily available, simple to administer, relatively inexpensive, with minimal side effects.
Pharmacology
| Tranexamic Acid | |
| Dose | Loading dose: 1 g over 10 minutes started within 3 hours of injury2 gram via slow IV Push* Maintenance: 1 g over the next 8 hours as a continuous infusion |
| Administration | Loading dose: administer undiluted Max rate:100 mg/minute For continuous IV infusions: dilute with compatible solutions and administer at a rate not to exceed 100 mg/minute |
| PK/PD | Distribution: Vd: IV: 9 to 12 L Protein binding: ~3%, primarily to plasminogen Half-life elimination: ~2 hours Excretion: Urine (>95% as unchanged drug) |
| Adverse Effects | Hypersensitivity reactions, ocular effects, seizures and myoclonus, thromboembolic effects, abdominal pain, headache, back pain |
Overview of Evidence
| Author, year | Design/ sample size | Intervention & Comparison | Outcome |
| Morrison, 2012 | ○ Observational (n=896) | ○ TXA 1g bolus + repeat prn vs placebo. | All-cause mortality overall within 48 hours and in hospital mortality significantly reduced with TXA |
| Roberts, 2013 | ○ Randomized placebo-controlled (n = 20,2011) | ○ TXA 1g bolus + 1g over 8 hours vs placebo | ○ All-cause mortality at 28 days was significantly reduced by TXA ○ Treatment within 1 hour and 1-3 hours from injury significantly reduced the risk of death due to bleeding |
| Sprigg, 2018 | ○ Randomized placebo-controlled (n= 2325) | ○ TXA 1 g bolus + 1g over 8 h infusion vs placebo | ○ Patients in the tranexamic acid group experienced a reduction in early deaths and serious adverse events, but not long term functional status |
| Roberts, 2019 | ○ Randomized, placebo-controlled (n=12737) | ○ TXA 1 g bolus + 1g over 8 hours vs placebo | ○ Treatment within 3 h of injury reduced head injury-related death. |
| Rowell, 2020 | ○ Double-blinded, randomized ( n= 966) | ● TXA 1 g bolus + 1 g 8-hour infusion vs 2 g bolus bolus + placebo infusion vs placebo bolus + placebo infusion | ○ No statistically significant difference in 28-day mortality, favorable neurologic function, 6 month disability rating score, or progression of intracranial hemorrhage |
| Roberts, 2020 | ○ Randomized placebo-controlled (n = 12,009) | ○ TXA 1 g + 3g infusion vs placebo | ○ No significant difference in death due to bleeding within 5 days |
| Bossers, 2021 | ● Prospective observational cohort (n = 1827) | ○ Pre-hospital TXA vs no TXA patients with TBI | ○ No association between TXA and mortality was found at 30 days ○ TXA was associated with increased mortality in patients with isolated TBI |
| Guyette, 2021 | ○ Double-blind, placebo-controlled, randomized ( n= 927) | ○ TXA 1 g bolus only vs TXA 1g + 1 g infusion vs TXA 1g bolus + 1g bolus + 1g infusion vs placebo bolus + placebo infusion | ○ Prehospital administration of tranexamic acid compared with placebo did not result in a lower rate of 30-day mortality in this population. ○ No differences were found in 24-hour mortality or in-hospital mortality |
| Mahmood, 2021 | ○ Randomized placebo-controlled (n = 1767) | ○ TXA 1 g bolus + 1 vs placebo | ○ No evidence that TXA prevents IPH expansion |
| Gruen, 2023 | ○ Double-blind, randomized, placebo-controlled (n = 1310) | ○ TXA 1 g bolus prior + infusion vs matched placebo | ○ No difference in survival with a favorable functional outcome at 6 months ○ No difference in 6 months mortality |
Conclusions
- Tranexamic acid has been studied in pre-hospital, hospital, and combat setting in patients who have sustained a traumatic injury
- Efficacy of tranexamic acid was demonstrated in some studies above, while other studies failed to show a significant difference in outcomes
- Dosing of tranexamic acid varied significantly in the above studies, however one dosing regimen has been widely adopted
- Tranexamic acid has minimal adverse effects, is relatively inexpensive, and readily available in many settings
References
- Rhee P, Joseph B, Pandit V, et al. Increasing trauma deaths in the United States. Ann Surg. 2014;260(1):13-21. doi:10.1097/SLA.0000000000000600
- Callcut RA, Kornblith LZ, Conroy AS, et al. The why and how our trauma patients die: A prospective Multicenter Western Trauma Association study. J Trauma Acute Care Surg. 2019;86(5):864-870. doi:10.1097/TA.0000000000002205
- Latif RK, Clifford SP, Baker JA, et al. Traumatic hemorrhage and chain of survival. Scand J Trauma Resusc Emerg Med. 2023;31(1):25. Published 2023 May 24. doi:10.1186/s13049-023-01088-8
- Hijazi N, Abu Fanne R, Abramovitch R, et al. Endogenous plasminogen activators mediate progressive intracerebral hemorrhage after traumatic brain injury in mice. Blood. 2015;125(16):2558-2567. doi:10.1182/blood-2014-08-588442
- Cai J, Ribkoff J, Olson S, et al. The many roles of tranexamic acid: An overview of the clinical indications for TXA in medical and surgical patients. Eur J Haematol. 2020;104(2):79-87. doi:10.1111/ejh.13348
- Morrison JJ, Dubose JJ, Rasmussen TE, Midwinter MJ. Military Application of Tranexamic Acid in Trauma Emergency Resuscitation (MATTERs) Study. Arch Surg. 2012;147(2):113-119. doi:10.1001/archsurg.2011.287
- Roberts I, Shakur H, Coats T, et al. The CRASH-2 trial: a randomised controlled trial and economic evaluation of the effects of tranexamic acid on death, vascular occlusive events and transfusion requirement in bleeding trauma patients. Health Technol Assess. 2013;17(10):1-79. doi:10.3310/hta17100
- Sprigg N, Flaherty K, Appleton JP, et al. Tranexamic acid for hyperacute primary IntraCerebral Haemorrhage (TICH-2): an international randomised, placebo-controlled, phase 3 superiority trial. Lancet. 2018;391(10135):2107-2115. doi:10.1016/S0140-6736(18)31033-X
- CRASH-3 trial collaborators. Effects of tranexamic acid on death, disability, vascular occlusive events and other morbidities in patients with acute traumatic brain injury
- Micromedex [Electronic version].Greenwood Village, CO: Truven Health Analytics. Retrieved January 17, 2021, from http://www.micromedexsolutions.com/
How to Fail the BCEMP Exam
The Board Certified Emergency Medicine Pharmacotherapy (BCEMP) exam, offered by the Board of Pharmacy Specialties, represents a significant milestone for healthcare professionals specializing in emergency medicine pharmacotherapy. This rigorous certification process is designed to validate a practitioner’s knowledge and skills, ensuring their capability to provide optimal medication therapy in emergency situations. While aiming for success is the natural course, today, we adopt a contrarian approach by highlighting the pitfalls that could lead to failure. This reverse-psychology method aims to illuminate the path towards effective preparation by understanding the common mistakes to avoid.
1. Misunderstanding the Exam’s Scope and Requirements
Understanding the full scope and requirements of the BCEMP exam is crucial for candidates aspiring to certify their expertise in emergency medicine pharmacotherapy. The Board of Pharmacy Specialties offers a detailed overview, including eligibility criteria, content areas, and a candidate’s guide on bpsweb.org, which serves as an essential resource for aligning preparation efforts with the exam’s demands. The exam encompasses a wide range of topics, from pharmacotherapy interventions to toxicological emergencies, requiring not just memorization but the ability to apply knowledge in complex clinical scenarios. Familiarity with these details ensures a targeted and effective study plan, addressing the depth of knowledge and breadth of topics expected.
Underestimating the breadth of topics covered in the BCEMP exam can lead to significant preparation gaps, potentially impacting exam performance. A narrow focus on certain areas while neglecting others can leave candidates ill-equipped to handle the diverse and complex questions posed. The comprehensive nature of the exam, designed to reflect the real-world challenges of emergency medicine, necessitates a thorough and well-rounded approach to study. By leveraging resources like the candidate’s guide from the Board of Pharmacy Specialties, candidates can avoid the pitfalls of underestimation and ensure a holistic preparation strategy that covers all necessary content areas.
2. Relying on Ineffective Study Techniques
Relying solely on ineffective study techniques such as cramming and passive reading can be a major pitfall in preparing for the BCEMP exam. These methods are particularly unsuitable for mastering the complex and detailed information required in emergency medicine pharmacotherapy. Cramming, or the intense absorption of material shortly before the exam, fails to facilitate the deep learning necessary for long-term retention of intricate concepts. Passive reading, without active engagement, doesn’t reinforce the material in a meaningful way, making it difficult to recall under exam pressure. recall under exam pressure. The “Eight Recommendations to Promote Effective Study Habits for Biology Students Enrolled in Online Courses” emphasize the value of active learning, even in online
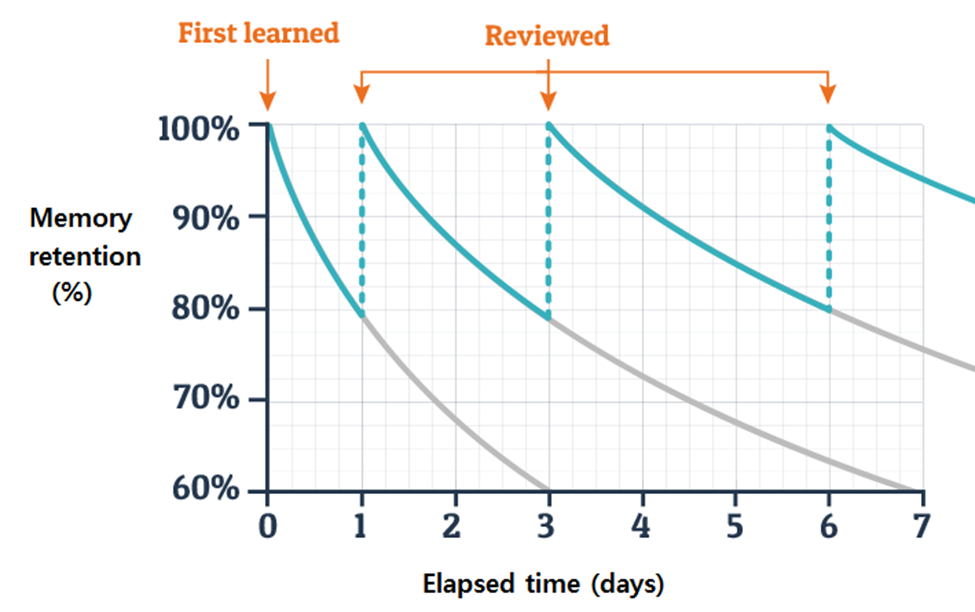
settings, suggesting that techniques fostering active engagement lead to more effective study habits. On the other hand, the benefits of spaced repetition, a study technique that involves reviewing material over increasing intervals, cannot be overstated. This method is grounded in the psychological principle of the spacing effect, which suggests that information is more easily recalled if learning sessions are spaced out over time. The Medium article “Importance of Spaced-Repetitions” highlights that spaced repetition significantly enhances long-term retention compared to massed practice (cramming), making it a superior strategy for complex subjects like pharmacotherapy. Additionally, the concept of the Ebbinghaus Forgetting Curve, detailed in “Ebbinghaus Forgetting Curve (Definition + Examples),” illustrates the natural decline of memory retention over time and how spaced repetition can counteract this effect. By incorporating these evidenced-based strategies into their study plan, candidates can greatly improve their grasp and retention of the extensive material covered in the BCEMP exam.
3. Overlooking Practice Exams and Question Banks
Overlooking the value of practice exams and question banks can be a critical misstep in preparing for the BCEMP exam. These tools are essential for familiarizing oneself with the exam’s structure and the variety of questions that may be encountered. A lack of exposure to the exam format and question types can lead to difficulties in navigating the actual test, potentially impacting performance. Incorporating practice materials into one’s study routine not only aids in understanding the exam’s layout but also helps in identifying weak areas that require additional focus.
Integrating practice exams and questions into the study schedule early and consistently is key to building confidence and competence. Engaging with a variety of questions, similar to those found in well-curated resources like PACUPrep’s Q-Bank, allows candidates to simulate the exam experience, enhancing their ability to manage time and approach questions effectively. This regular practice helps in cementing knowledge and honing test-taking strategies, making the actual exam environment more familiar and less intimidating. Through this disciplined approach, candidates can significantly improve their preparedness, paving the way for success in the BCEMP exam.
4. Poor Time Management
Poor time management in the context of BCEMP exam preparation can create significant barriers to success, primarily through the development of gaps in knowledge. Without a structured approach to studying, candidates risk spending too much time on certain topics while neglecting others, leading to an uneven grasp of the required material. This imbalance can be detrimental on exam day, where a comprehensive understanding across all areas is essential. Effective allocation of study time is crucial, ensuring that each topic is given due attention based on its complexity and the candidate’s familiarity with it.
To counteract this, adopting time management strategies can greatly enhance study efficiency. For instance, the Pomodoro Technique can be particularly effective in maintaining focus and preventing burnout. By dividing study sessions into 25-minute focused intervals followed by short breaks, candidates can improve retention and sustain longer periods of productive study. Additionally, the use of calendar apps to schedule study sessions and track important deadlines ensures a structured approach, covering all necessary topics systematically. During the exam, strategies such as quickly scanning all questions to allocate time effectively and keeping track of time to pace oneself can further optimize performance, ensuring that all questions are addressed within the allotted time.
5. Neglecting Mental and Physical Health
Neglecting mental and physical health during the preparation for the BCEMP exam can significantly undermine a candidate’s cognitive function and overall performance. The intense demands of studying for such a rigorous exam can lead to stress and sleep deprivation, which are known to impair memory, concentration, and decision-making abilities. Maintaining a healthy lifestyle, therefore, becomes not just a matter of personal well-being but a strategic component of exam preparation.
Adequate sleep is fundamental to cognitive processes, including the consolidation of memory, which is crucial when absorbing vast amounts of information. Similarly, effective stress management techniques such as regular exercise, mindfulness practices, or engaging in hobbies can mitigate the adverse effects of prolonged study sessions. These practices not only help in maintaining mental clarity and focus but also contribute to a more resilient and adaptable mindset, enabling candidates to tackle the challenges of the exam with greater composure and confidence. By prioritizing health and well-being, candidates can optimize their cognitive function, enhancing their ability to learn, retain, and apply knowledge effectively.
6. Studying in Isolation
Studying in isolation for the BCEMP exam can limit a candidate’s perspective and understanding, as it restricts the exchange of ideas, knowledge, and experiences that are vital for a comprehensive learning process. Engaging solely with the material without external input or discussion can lead to a narrow interpretation of complex topics and potentially overlook areas that might be crucial for the exam. The collaborative learning that occurs in group settings can expose candidates to diverse problem-solving approaches, clarify doubts through discussion, and reinforce learning through teaching others. To counteract the drawbacks of solitary study, candidates are encouraged to participate in study groups, professional forums, and seek mentorship.
7. Not Staying Updated with Current Practices
The field of emergency medicine pharmacotherapy is dynamic, with continuous advancements in treatment protocols, medication management, and clinical guidelines. Not incorporating the latest research findings, guidelines, and best practices into study materials for the BCEMP exam can lead to a knowledge base that is outdated and not reflective of current standards of care. This gap can be particularly detrimental in an exam setting that evaluates a candidate’s ability to apply contemporary, evidence-based practices in emergency medicine scenarios.
To ensure that study materials are current and comprehensive, candidates should regularly consult reputable medical journals in the field of emergency medicine and pharmacotherapy. These journals often publish the latest research, reviews, and consensus guidelines that can inform and update a candidate’s knowledge. Additionally, engaging in continuing education courses and participating in professional networks and associations can provide insights into emerging trends and consensus opinions in the field. These resources not only aid in preparing for the BCEMP exam but also contribute to a practitioner’s ongoing professional development, ensuring that their practice remains aligned with the highest standards of patient care in emergency medicine pharmacotherapy.
Conclusion: Embracing a Proactive and Balanced Approach to Exam Preparation
In preparing for the BCEMP exam, it’s crucial to avoid common pitfalls that can hinder success. Understanding the exam’s scope, avoiding ineffective study techniques, utilizing practice exams, managing time effectively, maintaining health, engaging with peers and mentors, and staying updated with current practices are all key to a well-rounded preparation strategy. Neglecting any of these areas can lead to gaps in knowledge, unnecessary stress, and ultimately, underperformance in the exam.
Embracing a proactive and balanced approach to studying is essential. This means not only covering all the necessary material but doing so in a way that promotes deep understanding and long-term retention. Active learning, effective time management, collaboration, and continuous learning are all part of a holistic study plan. The goal is not just to pass the BCEMP exam but to excel in the field of emergency medicine pharmacotherapy, ensuring that you are well-equipped to provide the highest level of care to patients in critical situations. By avoiding these common pitfalls and adopting a disciplined approach to preparation, candidates can position themselves for success, both in the exam and in their professional practice.
References
- American Board of Pharmacy Specialties. Pharmacotherapy: Specialty Certification Examination Content Outline. https://www.bpsweb.org/wp-content/uploads/bps-specialties/pharmacotherapy/PT_contentoutline.pdf. Accessed September 28, 2021.
- Dunlosky J, Rawson KA, Marsh EJ, Nathan MJ, Willingham DT. Improving students’ learning with effective learning techniques: promising directions from cognitive and educational psychology. Psychol Sci Public Interest. 2013;14(1):4-58. doi:10.1177/1529100612453266
- Brown PC, Roediger HL 3rd, McDaniel MA. Make It Stick: The Science of Successful Learning. Cambridge, MA: Belknap Press of Harvard University Press; 2014.
- Johnson M, Taubenheim A, Samar H, et al. Examining the impact of practice testing on learning and retention of medical information. Curr Pharm Teach Learn. 2020;12(9):1037-1045. doi:10.1016/j.cptl.2020.06.005
- Hartwig MK, Dunlosky J. Study strategies of college students: are self-testing and scheduling related to achievement? Psychon Bull Rev. 2012;19(1):126-134. doi:10.3758/s13423-011-0181-y
- McDaniel MA, Agarwal PK, Huelser BJ, McDermott KB, Roediger HL 3rd. Test-enhanced learning in a middle school science classroom: the effects of quiz frequency and placement. J Educ Psychol. 2011;103(2):399-414. doi:10.1037/a0021782
- Kornell N, Bjork RA. The promise and perils of self-regulated study. Psychon Bull Rev. 2007;14(2):219-224. doi:10.3758/bf03194055
- Chew SL. How to Get the Most Out of Studying Video Series. http://www.samford.edu/how-to-study/. Published 2011. Accessed September 28, 2021.
- Tuckman BW, Rapport MD. A 16-session time management intervention for college students with attention deficit hyperactivity disorder. Behav Modif. 2019;43(4):527-559. doi:10.1177/0145445518777735
- Dyrbye LN, Shanafelt TD, Sinsky CA, et al. Burnout among health care professionals: a call to explore and address this underrecognized threat to safe, high-quality care. NAM Perspectives. 2017;7(7). doi:10.31478/201707b
- Pagnini F, Bercovitz KE, Phillips D. Calm education: meta-analysis of mindfulness and emotion regulation strategies for teachers and students. Int J Stress Manag. 2018;25(4):364-376. doi>10.1037/str0000104
- Cohen S, Janicki-Deverts D, Miller GE. Psychological stress and disease. JAMA. 2007;298(14):1685-1687. doi:10.1001/jama.298.14.1685
- Krupat E, Richards JB, Sullivan AM, Fleenor TJ Jr, Schwartzstein RM. Assessing the effectiveness of case-based collaborative learning via randomized controlled trial. Acad Med. 2016;91(5):723-729. doi:10.1097/ACM.0000000000001044
- Karpicke JD, Blunt JR. Retrieval practice produces more learning than elaborative studying with concept mapping. Science. 2011;331(6018):772-775. doi:10.1126/science.1199327
- Singh N. Habituation, Memory, Spaced-Repetitions, Massed-Repetition. LeMe’24 Blog Post 4. March 7, 2024. Available from: https://medium.com/@nishchay.singh.23510074/habituation-memory-spaced-repetitions-massed-repetition-7640d4595429
- Ewell SN, Cotner S, Drake AG, Fagbodun S, Google A, Robinson L, Soneral P, Ballen CJ. 2022. Eight Recommendations to Promote Effective Study Habits for Biology Students Enrolled in Online Courses. J Microbiol Biol Educ. 23:e00260-21.
PROPHY-VAP Trial
Study To Review
One Sentence Summary
The PROPHY-VAP trial showed that a single dose of ceftriaxone can significantly reduce early-onset VAP in mechanically ventilated brain-injured patients, offering a potential change in clinical practice for VAP prevention.
Introduction
Methods
Results
Ventilator-associated pneumonia (VAP) is a significant concern in intensive care units (ICU), especially prevalent among brain-injured patients who are mechanically ventilated. With VAP incidence rates ranging from 22% to 71%, depending on the study, and brain injury being a notable independent risk factor, the prevention of this infection is paramount. Current standard of care includes a set of measures aiming to reduce the incidence of VAP; however, the challenge of early versus late onset VAP and the associated risk of multi-drug resistant organisms necessitate ongoing research and innovation in prophylactic strategies. The PROPHY-VAP trial is a pivotal study that explores the use of prophylactic antibiotics, specifically ceftriaxone, to prevent early-onset VAP in brain-injured patients. By addressing the controversial cut-off for early VAP onset in this population and considering the unique susceptibility profile of their infections, this trial holds significant importance for enhancing patient outcomes and refining ICU protocols.
PROPHY-VAP was a multicentre, randomized, double-blind, placebo-controlled trial conducted in nine French ICUs. The study enrolled comatose adult patients (Glasgow Coma Scale score ≤12) requiring mechanical ventilation post-acute brain injury. Patients were randomly assigned to receive either intravenous ceftriaxone 2 g or a placebo within 12 hours of tracheal intubation. The primary outcome was the incidence of early VAP (2nd to 7th day of mechanical ventilation). The study excluded patients with high death risk within 48 hours, previous hospitalizations for coma, contraindications to beta-lactams, and those receiving antibiotics for pre-existing infections.
- The PROPHY-VAP trial was conducted over a period spanning from October 14, 2015, to May 27, 2020, during which 345 patients were randomized in a 1:1 ratio to receive either ceftriaxone (171 patients) or placebo (174 patients). The study observed a marked reduction in the incidence of early VAP in the ceftriaxone group, with only 14% (23 patients) developing the infection compared to 32% (51 patients) in the placebo group, translating to a hazard ratio of 0.60. This significant decrease in early-onset VAP incidence, demonstrated in a double-blind, placebo-controlled setting, suggests that a single dose of ceftriaxone can be an effective prophylactic intervention in brain-injured patients requiring mechanical ventilation.
A detailed analysis of the patient demographics within the trial revealed that out of the 319 patients included in the analysis, 166 were men and 153 were women. Adjudication confirmed a total of 93 cases of VAP, of which 74 were early infections. Importantly, the study reported no increase in multi-drug resistant organisms or adverse effects attributable to the administration of ceftriaxone. These results indicate that the intervention was not only efficacious in reducing the incidence of early VAP but also safe for the patients, with no additional risk of fostering antibiotic resistance. The authors report that these findings provide a strong argument for the inclusion of a single dose of ceftriaxone in VAP prevention bundles for this patient population.
Conclusion
The study demonstrates that a single dose of ceftriaxone significantly reduces the risk of early VAP in brain-injured patients requiring mechanical ventilation, without adverse microbiological consequences. This finding supports the inclusion of an early ceftriaxone dose in VAP prevention protocols for brain-injured patients.
Impression
The PROPHY-VAP trial’s findings have sparked debate within the medical community, with practitioners expressing both interest in the potential benefits of ceftriaxone prophylaxis and concern regarding the broader implications of antibiotic use, such as the risk of over-diagnosis of VAP and the absence of data on late-onset VAP and resistant pathogens. These discussions underscore the necessity for further research and careful consideration before integrating these results into standard practice.
Further Readings
Piperacillin-tazobactam plus Vancomycin and Acute Kidney Injury by Caroline Rosario
Introduction
- Vancomycin and piperacillin-tazobactam are combined for broad-spectrum antibiotic coverage including MRSA and Pseudomonas in hospitalized patients.
- AKI, often as acute tubular necrosis, is a known complication of vancomycin, especially with higher doses and co-administration of nephrotoxic drugs.
- Piperacillin-tazobactam alone has minimal nephrotoxicity (<1%); its nephrotoxicity is usually due to acute interstitial nephritis.
- Reported AKI rates vary in literature based on AKI definition and target population.
- Both drugs affect OAT1/3 transporters in the kidney, which are crucial for creatinine clearance and are especially significant in patients with CKD.
Pharmacology
| Vancomycin | Piperacillin-tazobactam4 | |
| Dose | Depends on infection and PK/PD target General dosing for systemic infections: IV 15-20 mg/kg IV Q8-12H for systemic infections | Standard infusion: 3.375 g IV Q6H over 30 minAntipseudomonal: 4.5 g IV Q6-8H over 30 minExtended infusion: 4.5 g IV then 3.375-4.5 g over 4 hours Q8H |
| Administration | Administer IV over ≥60 minutes at concentrations ≤5 mg/mL to reduce the risk of vancomycin infusion reaction | Standard infusion: Infuse over 30 min Extended infusion: Infuse loading dose over 30 min, start maintenance dose four hours later infused over 4 hours |
| PK/PD | Negligible oral bioavailability T1/2 = 4-6 hours Renally eliminated (40-100% unchanged) AUC:MIC dependent kinetics, PK/PD target AUC/MIC ≥400 µg/mL; surrogate serum trough concentrations often used | T1/2 = 0.7-1.2 hours Renally eliminated (80% unchanged) Dose adjust at CrCl<40 T>MIC dependent kinetics, prolonged infusions enhance efficacy |
| Adverse Effects | Nephrotoxicity Ototoxicity Vancomycin-infusion reaction (flushing, hypotension, tachycardia) | GI upset (diarrhea, nausea, constipation) Headache Rash, pruritis |
| Drug Interactions and warnings | Substrate of OAT1/3 +/- Inducer of OAT1/3 ↑ nephrotoxicity: aminoglycosides, aspirin | Piperacillin: substrate and inhibitor of OAT1/3∆, Tazobactam: substrate of OAT1/3 Interactions: Probenecid (↑ piperacillin-tazobactam), Methotrexate (↑ methotrexate) |
| Compatibility | Compatible with dextrose, NS, LR Incompatible with lipid emulsion | LR: only the formulation containing EDTA is compatible for Y-site administration Not chemically stable in solutions containing sodium bicarbonate or solutions that significantly alter pH Cannot be added to blood products or albumin hydrolysates |
| Comments | Serum troughs are a poor proxy of 24-hour AUC, trough-guided regimens have been shown to exceed the target AUC in 60% of adults10 | Useful in the ED for anaerobic coverage in Grade III open fractures, pneumonia with lung abscess or empyema, and empiric antipseudomonal coverage in patients with risk factors |
Overview of Evidence
| Author, year | Design/ sample size | Intervention & Comparison | AKI definition | Outcome |
| Sanz et al., 2002 | Prospective, multi-center (n = 969) | Amikacin+cefepime vs. amikacin+piperacillin-tazobactam | ↑ SCr ≥50% from baseline | No difference in severe nephrotoxicity between amikacin+piperacillin-tazobactam vs. amikacin+cefepime |
| Karino et al., 2016 | Retrospective cohort and nested case-control studies (n = 320) | Vancomycin+piperacillin-tazobactam standard infusion vs. Vancomycin+piperacillin-tazobactam extended-infusion | RIFILE criteriaAKIN criteriaVancomycin consensus guideline definition | AKI occurred in 33% of patients receiving vancomycin+piperacillin-tazobactamUse of extended infusion piperacillin-tazobactam did not increase risk of AKI Highest daily incidence of AKI occurred on day 5 of combination therapy |
| Hammond et al., 2017 | Meta-analysis of 14 observational studies (n = 3549) | Vancomycin+piperacillin-tazobactam vs. vancomycin+any β-lactam or vancomycin alone | All included studies used one of the following: RIFLE criteriaAKIN criteria↑ SCr ≥100% or >0.5 mg/dL | Vancomycin+piperacillin-tazobactam greater association with AKI (aOR, 3.11; 95% CI, 1.77–5.47) Highest incidence of AKI in patients admitted to the ICU (OR 3.83 95% CI, 1.67-8.78) |
| Rutter et al., 2017 | Retrospective matched cohort (n = 4103) | Vancomycin+piperacillin-tazobactam vs. vancomycin+cefepime | RIFLE criteria | Vancomycin+piperacillin-tazobactam 2.18 times more likely to cause AKI vs. vancomycin+cefepime (95% CI, 1.64–2.94) Vancomycin doses between 3 and 4 g daily used, |
| Peyko et al., 2017 | Prospective observational cohort (n = 85) | Vancomycin+piperacillin-tazobactam vs. vancomycin+cefepime or vancomycin+meropenem | KDIGO | Incidence of AKI was higher in with vancomycin+piperacillin-tazobactam vs. vancomycin+cefepime or meropenem (37.3% vs. 7.7% P = .005) |
| Rutter and Burgess et al., 2017 | Retrospective matched cohort (n = 2448) | Vancomycin+piperacillin-tazobactam vs. Vancomycin+ampicillin-sulbactam | RIFLE criteria | Increased risk of AKI with vancomycin+piperacillin-tazobactam (aOR, 1.77; 95% CI, 1.26–2.46), no increased rate of AKI with vancomycin+ampicillin-sulbactamRates of AKI similar for piperacillin-tazobactam and ampicillin-sulbactam without vancomycin |
| Jeon et al., 2017 | Retrospective matched cohort (n = 5335) | Vancomycin+piperacillin-tazobactam vs. vancomycin+cefepime | ↑ SCr ≥0.3 mg/dL or ≥50% from baseline | Vancomycin+piperacillin-tazobactam associated with a higher risk of AKI vs. vancomycin-cefepime (aHR, 1.25; 95% CI, 1.11–1.42.) |
| Mousavi et al., 2017 | Retrospective matched cohort (n = 280) | Vancomycin+piperacillin-tazobactam standard infusion vs. Vancomycin+piperacillin-tazobactam extended-infusion | RIFLE criteriaAKIN criteria | Similar rate of AKI between vancomycin+piperacillin-tazobactam standard infusion vs. vancomycin+piperacillin-tazobactam extended-infusionHigher vancomycin troughs were observed in the extended infusion group |
| Miano et al., 2022 | Prospective, observational | Vancomycin+piperacillin-tazobactam vs. vancomycin+cefepime for ≥48 hours | ↑ SCr vs. ↑ Cystatin C vs. ↑ BUN | Vancomycin + piperacillin-tazobactam ➡️ ↑ serum creatinine-defined AKI, but no change in cystatin C, BUN, or AKI outcomes (dialysis/mortality).Indicates vancomycin + piperacillin-tazobactam AKI may be pseudotoxicity. |
| Qian et al, 2023 (ACORN Trial) | Randomized controlled Trial N=2511 | Vancomycin+piperacillin-tazobactam vs. vancomycin+cefepime | KDIGO ↑ SCr ≥0.3 mg/dL or ≥50% from baseline | The highest stage of acute kidney injury or death was not significantly different between the cefepime group and the piperacillin-tazobactam groupThe incidence of major adverse kidney events at day 14 did not differ between groups (124 patients [10.2%] in the cefepime group vs 114 patients [8.8%] in the piperacillintazobactam group~77% of each concurrently received vancomycin |
RIFLE, AKIN and KDIGO definitions of AKI are based upon ↑ in serum creatinine or ↓ in urine output
Conclusions
- Since 2011, evidence indicates combined vancomycin+ piperacillin-tazobactam may be nephrotoxic.
- Most studies were retrospective, defining nephrotoxicity by creatinine-based AKI.
- Recent data show this AKI definition doesn’t align with severe AKI outcomes (hemodialysis/mortality).
- Non-tubular secretion biomarkers (Cystatin C, BUN) didn’t show the same AKI increase.
- Despite >50 studies linking the drug combo with AKI, some expert report true renal risk is likely minimal.
- In emergencies, timely antibiotic use is vital; nephrotoxicity concerns shouldn’t delay this combo, especially for short use.
References
- Micromedex [Electronic version].Greenwood Village, CO: Truven Health Analytics. Retrieved October 4, 2023, from http://www.micromedexsolutions.com/
- VANCOMYCIN HYDROCHLORIDE [package insert]. Rockford, IL: Mylan Institutional LLC; Jul, 2018.
- Blair M, Côté JM, Cotter A, Lynch B, Redahan L, Murray PT. Nephrotoxicity from Vancomycin Combined with Piperacillin-Tazobactam: A Comprehensive Review. Am J Nephrol. 2021;52(2):85-97. doi: 10.1159/000513742.
- Pill MW, O’Neill CV, Chapman MM, Singh AK. Suspected acute interstitial nephritis induced by piperacillin-tazobactam. Pharmacotherapy. 1997 Jan-Feb;17(1):166-9..
- Li H, Yang Q, Gui M, Ding L, Yang L, Sun H, Li Z. Changes of renal transporters in the kinetic process of VCM-induced nephrotoxicity in mice. Toxicol Res (Camb). 2021 Jun 9;10(4):687-695. doi: 10.1093/toxres/tfab048. PMID: 34484661; PMCID: PMC8403606.
- Giuliano CA, Patel CR, Kale-Pradhan PB. Is the Combination of Piperacillin-Tazobactam and Vancomycin Associated with Development of Acute Kidney Injury? A Meta-analysis. Pharmacotherapy. 2016 Dec;36(12):1217-1228. doi: 10.1002/phar.1851.
- Boucher, H. (2023) Piperacillin-tazobactam, Sanford Guide Web Edition. Available at: https://webedition.sanfordguide.com/en/drug-information/antibacterial-agents/penicillins/anti-pseudomonal-penicillins/piperacillin-tazobactam (Accessed: 12 October 2023).
- Yang S, Liu Z, Wang C, Wen S, Meng Q, Huo X, Sun H, Ma X, Peng J, He Z, Liu K. Piperacillin enhances the inhibitory effect of tazobactam on β-lactamase through inhibition of organic anion transporter 1/3 in rats. Asian J Pharm Sci. 2019 Nov;14(6):677-686. doi: 10.1016/j.ajps.2018.11.003.
- Landersdorfer CB, Kirkpatrick CM, Kinzig M, Bulitta JB, Holzgrabe U, Sörgel F. Inhibition of flucloxacillin tubular renal secretion by piperacillin. Br J Clin Pharmacol. 2008 Nov;66(5):648-59. doi: 10.1111/j.1365-2125.2008.03266.x.
- Neely MN, Youn G, Jones B, Jelliffe RW, Drusano GL, Rodvold KA, Lodise TP. Are vancomycin trough concentrations adequate for optimal dosing? Antimicrob Agents Chemother. 2014;58(1):309-16. doi: 10.1128/AAC.01653-13.
- Alvarez-Arango S, Ogunwole SM, Sequist TD, Burk CM, Blumenthal KG. Vancomycin Infusion Reaction – Moving beyond “Red Man Syndrome”. N Engl J Med. 2021 Apr 8;384(14):1283-1286. doi: 10.1056/NEJMp2031891. Epub 2021 Apr 3.
- Vallon V, Eraly SA, Rao SR, Gerasimova M, Rose M, Nagle M, Anzai N, Smith T, Sharma K, Nigam SK, Rieg T. A role for the organic anion transporter OAT3 in renal creatinine secretion in mice. Am J Physiol Renal Physiol. 2012 May 15;302(10):F1293-9. doi: 10.1152/ajprenal.00013.2012. Epub 2012 Feb 15. PMID: 22338083; PMCID: PMC3362066.
- Sanz MA, López J, Lahuerta JJ, Rovira M, Batlle M, Pérez C, Vázquez L, Julià A, Palau J, Gutiérrez M, Capote FJ, Ramos F, Benlloch L, Larrea L, Jarque I; Spanish PETHEMA Group. Cefepime plus amikacin versus piperacillin-tazobactam plus amikacin for initial antibiotic therapy in haematology patients with febrile neutropenia: results of an open, randomized, multicentre trial. J Antimicrob Chemother. 2002 Jul;50(1):79-88. doi: 10.1093/jac/dkf087. PMID: 12096010.
- Watkins RR, Deresinski S. Increasing Evidence of the Nephrotoxicity of Piperacillin/Tazobactam and Vancomycin Combination Therapy-What Is the Clinician to Do? Clin Infect Dis. 2017 Nov 29;65(12):2137-2143. doi: 10.1093/cid/cix675.
- Karino S, Kaye KS, Navalkele B, Nishan B, Salim M, Solanki S, Pervaiz A, Tashtoush N, Shaikh H, Koppula S, Martin ET, Mynatt RP, Murray KP, Rybak MJ, Pogue JM. Epidemiology of Acute Kidney Injury among Patients Receiving Concomitant Vancomycin and Piperacillin-Tazobactam: Opportunities for Antimicrobial Stewardship. Antimicrob Agents Chemother. 2016 May 23;60(6):3743-50. doi: 10.1128/AAC.03011-15.
- Hammond DA, Smith MN, Li C, Hayes SM, Lusardi K, Bookstaver PB. Systematic Review and Meta-Analysis of Acute Kidney Injury Associated with Concomitant Vancomycin and Piperacillin/tazobactam. Clin Infect Dis. 2017 Mar 1;64(5):666-674. doi: 10.1093/cid/ciw811. Epub 2016 Dec 10. PMID: 27940946.
- Rutter WC, Cox JN, Martin CA, Burgess DR, Burgess DS. Nephrotoxicity during Vancomycin Therapy in Combination with Piperacillin-Tazobactam or Cefepime. Antimicrob Agents Chemother. 2017 Jan 24;61(2):e02089-16. doi: 10.1128/AAC.02089-16. Erratum in: Antimicrob Agents Chemother. 2017 Mar 24;61(4): PMID: 27895019; PMCID: PMC5278703.
- Peyko V, Smalley S, Cohen H. Prospective Comparison of Acute Kidney Injury During Treatment With the Combination of Piperacillin-Tazobactam and Vancomycin Versus the Combination of Cefepime or Meropenem and Vancomycin. J Pharm Pract. 2017 Apr;30(2):209-213. doi: 10.1177/0897190016628960.
- Rutter WC, Burgess DS. Acute Kidney Injury in Patients Treated with IV Beta-Lactam/Beta-Lactamase Inhibitor Combinations. Pharmacotherapy. 2017 May;37(5):593-598. doi: 10.1002/phar.1918.
- Jeon N, Staley B, Klinker KP, Hincapie Castillo J, Winterstein AG. Acute kidney injury risk associated with piperacillin/tazobactam compared with cefepime during vancomycin therapy in hospitalised patients: a cohort study stratified by baseline kidney function. Int J Antimicrob Agents. 2017 Jul;50(1):63-67. doi: 10.1016/j.ijantimicag.2017.02.023.
- Mousavi M, Zapolskaya T, Scipione MR, Louie E, Papadopoulos J, Dubrovskaya Y. Comparison of Rates of Nephrotoxicity Associated with Vancomycin in Combination with Piperacillin-Tazobactam Administered as an Extended versus Standard Infusion. Pharmacotherapy. 2017 Mar;37(3):379-385. doi: 10.1002/phar.1901. E
- Miano TA, Hennessy S, Yang W, Dunn TG, Weisman AR, Oniyide O, Agyekum RS, Turner AP, Ittner CAG, Anderson BJ, Wilson FP, Townsend R, Reilly JP, Giannini HM, Cosgriff CV, Jones TK, Meyer NJ, Shashaty MGS. Association of vancomycin plus piperacillin-tazobactam with early changes in creatinine versus cystatin C in critically ill adults: a prospective cohort study. Intensive Care Med. 2022 Sep;48(9):1144-1155. doi: 10.1007/s00134-022-06811-0.
- Evans L, Rhodes A, Alhazzani W, Antonelli M, Coopersmith CM, French C, Machado FR, Mcintyre L, Ostermann M, Prescott HC, Schorr C, Simpson S, Wiersinga WJ, Alshamsi F, Angus DC, Arabi Y, Azevedo L, Beale R, Beilman G, Belley-Cote E, Burry L, Cecconi M, Centofanti J, Coz Yataco A, De Waele J, Dellinger RP, Doi K, Du B, Estenssoro E, Ferrer R, Gomersall C, Hodgson C, Møller MH, Iwashyna T, Jacob S, Kleinpell R, Klompas M, Koh Y, Kumar A, Kwizera A, Lobo S, Masur H, McGloughlin S, Mehta S, Mehta Y, Mer M, Nunnally M, Oczkowski S, Osborn T, Papathanassoglou E, Perner A, Puskarich M, Roberts J, Schweickert W, Seckel M, Sevransky J, Sprung CL, Welte T, Zimmerman J, Levy M. Surviving sepsis campaign: international guidelines for management of sepsis and septic shock 2021. Intensive Care Med. 2021 Nov;47(11):1181-1247. doi: 10.1007/s00134-021-06506-y.
- Qian ET, Casey JD, Wright A, Wang L, Shotwell MS, Siemann JK, Dear ML, Stollings JL, Lloyd BD, Marvi TK, Seitz KP, Nelson GE, Wright PW, Siew ED, Dennis BM, Wrenn JO, Andereck JW, Han JH, Self WH, Semler MW, Rice TW; Vanderbilt Center for Learning Healthcare and the Pragmatic Critical Care Research Group. Cefepime vs Piperacillin-Tazobactam in Adults Hospitalized With Acute Infection: The ACORN Randomized Clinical Trial. JAMA. 2023 Oct 24;330(16):1557-1567. doi: 10.1001/jama.2023.20583. PMID: 37837651; PMCID: PMC10576861.
Seizure Prophylaxis in Traumatic Brain Injury by Jordan Spurling
Introduction
- Traumatic brain injury (TBI) is a leading cause of death and disability in the United States.
- The Brain Trauma Foundation updated its guidelines for the management of severe TBI in 2016; however, there remains a lack of randomized clinical trials addressing many aspects of care in TBI patient.
- The incidence of early post-traumatic seizures may be as high as 30 percent in patients with severe TBI
- Antiseizure medications in acute management of TBI has been shown to reduce incidence of early seizures but has not been shown to prevent later development of epilepsy
- Prevention of early seizures is beneficial in order to prevent status epilepticus, further aggravating systemic injury.
- The Brain Trauma Foundation guidelines recommend phenytoin for early post-traumatic seizures for 7 days following injury, however levetiracetam is commonly used in this setting.
Pharmacology
| Phenytoin | Valproic Acid | Levetiracetam | Lacosamide | ||
| Dose | Loading dose: 17 to 20 mg/kg IV (max dose 2 g) Maintenance dose: 100 mg every 8 hours or 5 mg/kg/day divided q8h (individual doses not to exceed 400 mg) Duration not to exceed 7 days | 10 – 15 mg/kg/day | Loading dose: 20 mg/kg IV infused over 5-20 min Maintenance dose: 1 g IV over 15 min every 12 hours for 7 days (may be increased to 1.5 g q12) | 50 – 100 mg IV twice daily May give loading dose of 200 mg | |
| Administration | IV piggyback rate of ≤50 mg/minute | IV piggyback over 60 minutes at a rate ≤20 mg/minute | IV push or piggyback over 5-20 min | Bolus: May be administered undiluted at ≤80 mg/minute Infusion: over 30 to 60 minutes | |
| PK/PD | Onset: 30 min – 1 hour Half-life:10 to 12 hours. | Peak: <1 hour Half-life:9 to 19 hours | Peak: 5-30 minutes Half-life: 6-8 hours | Peak: < 1 hour Half-life: ~13 hours | |
| Adverse Effects | Hematologic effects, cardiovascular effects, CNS effects, gingival hyperplasia, hepatotoxicity | CNS effects, hematologic effects, hepatotoxicity, encephalopathy, pancreatitis | CNS depression, hypersensitivity reactions, psychiatric and behavioral abnormalities, increased blood pressure, asthenia | Cardiac arrhythmias including bradycardia, AV block, CNS effects | |
| Warnings | Vesicant, acute toxicity | Not recommended for post-traumatic seizure prophylaxis in patients with acute head trauma | Caution in renal impairment. | Administer loading doses under medical supervision due to increased incidence of CNS adverse reactions | |
Guideline Recommendation
| Journal | Recommendations | |
| Guidelines for the Management of Severe Traumatic Brain Injury, Fourth Edition – 2017 | Phenytoin is recommended to decrease the incidence of early PTS (within 7 d of injury), when the overall benefit is thought to outweigh the complications associated with treatment. There is insufficient evidence to recommend levetiracetam compared with phenytoin regarding efficacy in preventing early post-traumatic seizures and toxicity. | |
Overview of Evidence
| Author, year | Design/ sample size | Intervention & Comparison | Outcome |
| Temkin, 1990 | A randomized, double-blind study N = 404 | Phenytoin vs Placebo | Within the first week 3.6% of phenytoin patients experienced seizure compared to 14.2% (p<0.001) Between day 8-1 year 21.5% of patients in phenytoin group experienced seizure compared to 15.7% in placebo group Phenytoin is effective in reducing seizures within the first 7 days after severe head injury |
| Young, 2004 | Randomized, Double-Blinded, Placebo- Controlled Trial in pediatric patients (age < 16 yo) N = 102 | Phenytoin vs Placebo for prevention of early posttraumatic seizures | During the 48-hour observation period, 3 of 46 (7%) patients in the phenytoin group and 3 of 56 (5%) patients in the placebo group experienced a posttraumatic seizure. No significant difference in survival or neurologic outcome between the two groups. Phenytoin did not significantly reduce the rate of posttraumatic seizures at 48 hours, neurologic outcomes, or overall survival at 30 days. |
| Jones, 2008 | Prospective, single-center trial N = 32 | Phenytoin vs Levetiracetam in patients with severe TBI (GCS 3-8) | Patients treated with levetiracetam and phenytoin had equivalent incidence of seizure activity (p = 0.556) Patients receiving levetiracetam had a higher incidence of abnormal EEG findings (p = 0.003). Levetiracetam is as effective as phenytoin in preventing early posttraumatic seizures but is associated with an increased seizure tendency on EEG |
| Temkin, 1990 | A randomized, double-blind study N = 404 | Phenytoin vs Placebo | Within the first week 3.6% of phenytoin patients experienced seizure compared to 14.2% (p<0.001) Between day 8-1 year 21.5% of patients in phenytoin group experienced seizure compared to 15.7% in placebo group Phenytoin is effective in reducing seizures within the first 7 days after severe head injury |
| Szaflarski, 2009 | Prospective, single-center, randomized, single-blinded comparative trial N = 52 | Levetiracetam vs Phenytoin in patients with severe traumatic brain injury (sTBI) or subarachnoid hemorrhage | Levetiracetam patients experienced better long-term outcomes than those on phenytoin. No differences between groups in seizure occurrence during cEEG (levetiracetam 5/34 vs. phenytoin 3/18; P = 1.0) or at 6 months (levetiracetam 1/20 vs. phenytoin 0/14; P = 1.0), or mortality (levetiracetam 14/34 vs. phenytoin 4/18; P = 0.227). Lower frequency of worsened neurological status (P = 0.024), and gastrointestinal problems (P = 0.043) in levetiracetam group Levetiracetam improved long-term outcomes of compared to phenytoin with less ADRs and may be an alternative. |
| Chi-yuan, 2010 | Retrospective, cohort study N = 171 | Sodium Valproate vs Placebo in early posttraumatic seizures in traumatic brain injury (TBI) patients. | No patients who received sodium valproate treatment experienced seizures; however, this was not statistically significant. Sodium valproate is effective in decreasing the risk of early posttraumatic seizures in severe TBI patients |
| Inaba, 2012 | Prospective, comparative study N = 1,191 | Levetiracetam vs Phenytoin for prevention of early post-traumatic seizures | No difference in seizure rate (1.5% vs.1.5%, p = 0.997) No difference between levetiracetam and phenytoin in the prevention of early post traumatic seizures, mortality or ADRs in patients following TBI. |
| Caballero, 2013 | Multicenter retrospective analysis N = 90 | Phenytoin vs Levetiracetam in TBI with at least one day of EEG monitoring | Prevalence of EEG-confirmed seizure activity was similar between the levetiracetam and phenytoin groups (28% vs 29%; p = .99). The median daily cost of levetiracetam therapy was $43 compared to $55 for phenytoin therapy and monitoring (p = .08). Levetiracetam may be an alternative treatment option for seizure prevention inTBI patients in the ICU while also providing lower costs for drug therapy and monitoring. |
| Kruer, 2013 | Retrospective observational study N = 109 | Phenytoin vs Levetiracetam in patients with a TBI and GCS < 8. | 79 out of 81 (98%) patients admitted between 2000 and 2007 received PHT, whereas 18 of 28 (64%) patients admitted between 2008 and 2010 received LEV. 1 patient out of 89 receiving phenytoin had a posttraumatic seizure and 1 patient out of 20 recieving levetiracetam experiences a posttraumatic seizure Only 2 patients experienced posttraumatic seizure after receiving AED, indicating low incidence of posttraumatic seizures. |
| Gabriel, 2014 | Single-center, prospective cohort analysis N = 19 | Phenytoin vs Levetiracetam after severe TBI | No difference in Glasgow Outcome Scale–Extended score assessed ≥6 months after injury No difference in early seizures (p = 0.53) or late seizures (p = 0.53) Higher days with fever experienced in the hospital in the phenytoin group. Long-term functional outcome in patients who experienced a TBI was not affected by treatment with PHT or LEV. |
| Khan, 2016 | Randomized controlled trial N = 154 | Phenytoin vs Levetiracetam in patients with moderate to severe head trauma | Phenytoin was effective in preventing early post traumatic seizures in 73 of 77 patients (94.8%) Levetiracetam effectively controlled seizures in 70 of 77 patients (90.95%) cases No statistically significant difference in the efficacy of Phenytoin and Levetiracetam in prophylaxis of early post-traumatic seizures in moderate to severe traumatic brain injury. |
Conclusions
- The Brain Trauma Foundation guidelines recommend phenytoin for early post-traumatic seizures for 7 days following injury, however levetiracetam is commonly used in this setting.
- In recent studies, lacosamide and levetiracetam showed no difference compared to phenytoin in prevention of early post-traumatic seizures following TBI
- Less side effects were associated with levetiracetam and lacosamide compared to phenytoin when used in seizure prophylaxis in TBI.
References
- Micromedex [Electronic version].Greenwood Village, CO: Truven Health Analytics. Retrieved October 17, 2023, from http://www.micromedexsolutions.com/
- Carney N, Totten AM, O’Reilly C, et al. Guidelines for the Management of Severe Traumatic Brain Injury, Fourth Edition. Neurosurgery. 2017;80(1):6-15. doi:10.1227/NEU.0000000000001432
- Frey LC. Epidemiology of Posttraumatic Epilepsy: A critical review. Epilepsia. 2003;44(s10):11-17. doi:10.1046/j.1528-1157.44.s10.4.x
- Micromedex [Electronic version].Greenwood Village, CO: Truven Health Analytics. Retrieved October 13, 2023, from http://www.micromedexsolutions.com/
- Temkin NR, Dikmen SS, Wilensky AJ, Keihm J, Chabal S, Winn HR. A randomized, double-blind study of phenytoin for the prevention of post-traumatic seizures. N Engl J Med. 1990;323(8):497-502. doi:10.1056/NEJM199008233230801
- Young KD, Okada PJ, Sokolove PE, et al. A randomized, double-blinded, placebo-controlled trial of phenytoin for the prevention of early posttraumatic seizures in children with moderate to severe blunt head injury. Annals of Emergency Medicine. 2004;43(4):435-446. doi:10.1016/j.annemergmed.2003.09.016
- Jones KE, Puccio AM, Harshman KJ, et al. Levetiracetam versus phenytoin for seizure prophylaxis in severe traumatic brain injury. Neurosurg Focus. 2008;25(4):E3. doi:10.3171/FOC.2008.25.10.E3
- Szaflarski JP, Lindsell CJ, Zakaria T, Banks C, Privitera MD. Seizure control in patients with idiopathic generalized epilepsies: EEG determinants of medication response. Epilepsy Behav. 2010;17(4):525-530. doi:10.1016/j.yebeh.2010.02.005
- Ma CY, Xue YJ, Li M, Zhang Y, Li GZ. Sodium valproate for prevention of early posttraumatic seizures. Chin J Traumatol. 2010;13(5):293-296.
- Inaba K, Menaker J, Branco BC, et al. A prospective multicenter comparison of levetiracetam versus phenytoin for early posttraumatic seizure prophylaxis. J Trauma Acute Care Surg. 2013;74(3):766-773. doi:10.1097/TA.0b013e3182826e84
- Caballero GC, Hughes DW, Maxwell PR, Green K, Gamboa CD, Barthol CA. Retrospective analysis of levetiracetam compared to phenytoin for seizure prophylaxis in adults with traumatic brain injury. Hosp Pharm. 2013;48(9):757-761. doi:10.1310/hpj4809-757
- Kruer RM, Harris LH, Goodwin H, et al. Changing trends in the use of seizure prophylaxis after traumatic brain injury: A shift from phenytoin to Levetiracetam. Journal of Critical Care. 2013;28(5). doi:10.1016/j.jcrc.2012.11.020
- Gabriel WM, Rowe AS. Long-term comparison of GOS-E scores in patients treated with phenytoin or levetiracetam for posttraumatic seizure prophylaxis after traumatic brain injury. Ann Pharmacother. 2014;48(11):1440-1444. doi:10.1177/1060028014549013
- Khan SA, Bhatti SN, Khan AA, et al. Comparison Of Efficacy Of Phenytoin And Levetiracetam For Prevention Of Early Post Traumatic Seizures. J Ayub Med Coll Abbottabad. 2016;28(3):455-460.
- Kwon YH, Wang H, Denou E, et al. Modulation of Gut Microbiota Composition by Serotonin Signaling Influences Intestinal Immune Response and Susceptibility to Colitis. Cell Mol Gastroenterol Hepatol. 2019;7(4):709-728. doi:10.1016/j.jcmgh.2019.01.004
Penicillin Allergy Cross Reactivity
Introduction
- Only 0.5% to 2% of patients with a documented penicillin allergy that are administered a penicillin will exhibit a hypersensitivity reaction, usually presenting as a rash or hives.
- True IgE-mediated penicillin allergies that cause anaphylaxis are rare.
- An IgE-mediated penicillin allergy can diminish over time, as 80% of patients become tolerant after a decade.
- Patients with a documented penicillin allergy may be inappropriately exposed to alternative antibiotics, resulting in increased treatment failures, adverse effects, and antimicrobial resistance.
- Penicillins, cephalosporins, and carbapenems all share a beta-lactam core structure, thus raising the potential for cross-reactivity among these agents.
Pharmacology
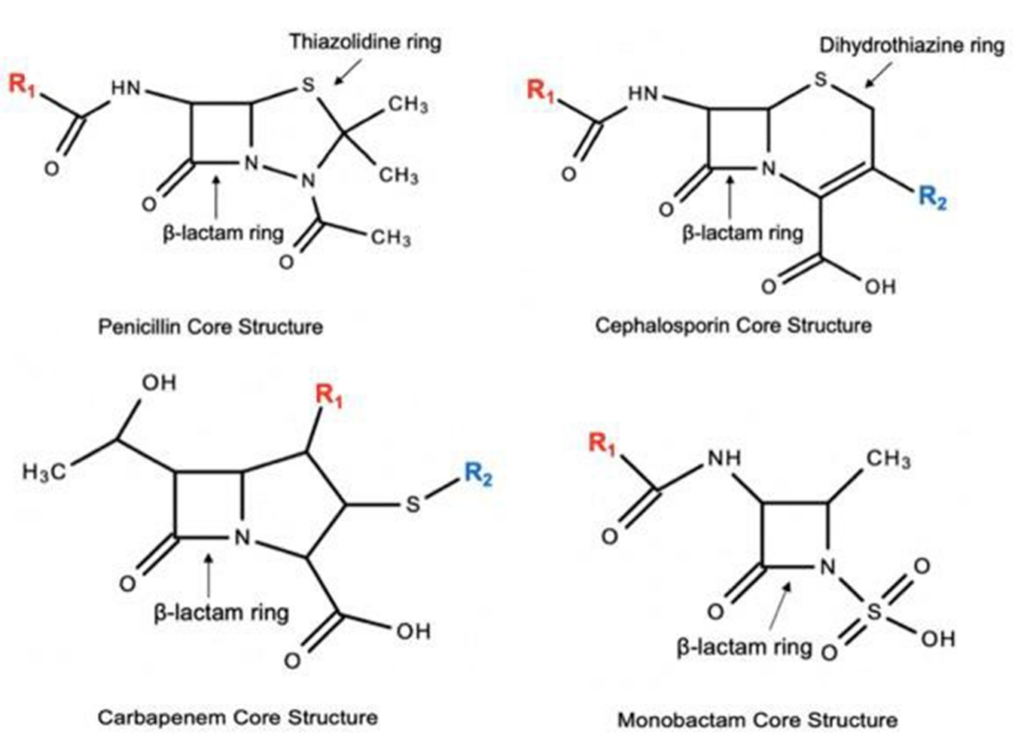
- The following drugs in each group may have cross-reactivity to each other due to similar side chains
- Cross-reactivity between penicillins and cephalosporins is about 2%
- Cefazolin is NOT likely to cross react with penicillin (side chains NOT similar)
- Cross-reactivity with monobactams (i.e. aztreonam) is negligible
- Cross-reactivity between penicillins and carbapenems is <1%
| Group 1 | Group 2 | Group 3 | Group 4 |
| Penicillin Cefoxitin Cefuroxime | Amoxicillin Ampicillin Cefaclor Cephalexin Cefadroxil | Ceftriaxone Cefotaxime Cefuroxime Cefepime Cefpodoxime Ceftaroline | Aztreonam Ceftolazane Ceftazidime |
Overview of Evidence
| Author | Design | Intervention & Comparison | Outcome | |
| Why Cross-Reactivity? | ||||
| Nagakura, 1990 Mayorga, 1995 | Animal study | -Studied antibodies formed when animals were immunized with protein-beta-lactam conjugates | -92% of the antibodies recognized an epitope in which the side chain was the main constituent -The side chain is the most important determinant in penicillin immunogenicity | |
| Cephalosporins | ||||
| Goodman, 2001 | Retrospective review (n=2933) | -Orthopedic patients with penicillin allergy receiving cefazolin prior to a procedure | Only 1 patient may have had an allergic reaction to cefazolinCross-reactivity rate with cefazolin was 0.33% | |
| Daulat, 2004 | Retrospective review (n=606) | -Patients with penicillin allergy receiving cephalosporins -42% 1st gen., 21% 2nd gen., and 37% 3rd or 4th gen. cephalosporins | Only 1 patient had an allergic reaction that was documented as worsening of underlying eczema after being placed on cefazolinCross-reactivity was 0.17% | |
| Apter, 2006 | Retrospective review (n=3920) | -Patients with a prescription for penicillin followed by a prescription for a cephalosporin -Identified allergic-like events within 30 days after each prescription | Only 43 patients who experienced an allergic- like reaction after both penicillin and cephalosporinCross-reactivity rate was 1.1%70% of these patients just had urticariaThe risk of anaphylaxis to cephalosporins was only 0.001% | |
| Romano, 2018 | Prospective review (n=252) | Prospective study of 252 subjects with IgE-mediated hypersensitivity to penicillins – Serum specific IgE assays for cefaclor and skin tests for 10 cephalosporins -Oral challenges with cefuroxime axetil, ceftriaxone, cefaclor, and cefadroxil for subjects with negative skin tests | 99 subjects (39.3%) had positive allergy tests for cephalosporins 95 subjects (37.7%) were positive to aminocephalosporins and/or cefamandole, which share side chains with penicillins All 244 subjects who underwent challenges with cefuroxime axetil and ceftriaxone tolerated them 7 subjects reacted to cefaclor or cefadroxil | |
| Carbapenems | ||||
| Romano, 2006 | Prospective study (n=112) | -Skin tested to penicillins and then skin tested to imipenem -If skin test to imipenem was negative, then challenged with IM dose | Only 1 patient of the penicillin skin-test positive patients had a positive skin test to imipenemCross-reactivity rate was 0.9%None of the 110 patients with a negative imipenem skin test that underwent IM challenge had a reaction | |
| Romano, 2007 | Prospective study (n=104) | -Skin tested to penicillins and then skin tested to meropenem -If skin test to imipenem was negative, then challenged with IV dose | Only 1 patient of the penicillin skin-test positive patients had a positive skin test to meropenemCross-reactivity rate was 1%All 103 patients with a negative meropenem skin test tolerated the IV challenge | |
| Atanaskovic- Markovic, 2008 | Prospective study (n=108) | -Children with penicillin allergy were skin tested to penicillin and meropenem -If skin test to meropenem was negative, then challenged with IV dose | Only 1 patient with a positive penicillin test reacted to the meropenem skin testCross-reactivity rate was 0.9%All 107 patients with a negative meropenem skin test tolerated the IV challenge | |
| Sánchez de Vicente, 2020 | Prospective study (n=137) | Tolerance testing for cephalosporins and carbapenems in patients with confirmed penicillin allergy | 0/46 patients showed positive skin tests for imipenem. 0.79% (1/137) patients showed a positive skin test for cefuroxime.0.79% (1/137) patients showed a positive skin test for ceftriaxone. | |
Conclusions
- True penicillin allergies are less common than reported, and anaphylaxis is uncommon.
- Cross-reactivity among penicillins and cephalosporins is attributed to similarity in side chains.
- Cephalosporin cross-reactivity with penicillins is much lower than reported in early studies partly due to contamination of study drugs with penicillin.
- Cross-reactivity between cephalosporins is about 2% and with carbapenems is <1%
References
- Apter AJ, Kinman JL, Bilker WB, et al. Is There Cross-Reactivity Between Penicillins and Cephalosporins? Am J Med. 2006;119(4):354e11-19.
- Atanaskovic-Markovic M, Gaeta F, Medjo B, Viola M, Nestorovic B, Romano A. Tolerability of Meropenem in Children with IgE-Mediated Hypersensitivity to Penicillins. Allergy. 2008;63:237-240.
- Blumenthal KG, Shenoy ES, Wolfson AR, et al. Addressing Inpatient Beta-Lactam Allergies: A Multihospital Implementation. J Allergy Clin Immunol Pract. 2017;5(3):616-625.
- Blumenthal KG, Huebner EM, Fu X, et al. Risk-Based Pathway for Outpatient Penicillin Allergy Evaluations. J Allergy Clin Immunol Pract. 2019;7(7):2411-2414.
- Campagna JD, Bond MC, Schabelman E, Hayes BD. The Use of Cephalosporins in Penicillin-Allergic Patients: A Literature Review. J Emerg Med. 2012;42(5):612-620.
- Chaudry SB, Veve MP, Wagner JL. Cephalosporins: A Focus on Side Chains and Beta-Lactam Cross-Reactivity. Pharmacy. 2019;7:1-16.
- Daulat S, Solensky R, Earl HS, Casey W, Gruchalla RS. Safety of Cephalosporin Administration to Patients with Hstories of Penicillin Allergy. J Allergy Clin Immunol Pract. 2004;113(6):1220-1222.
- DePestel DD, Benninger MS, Danziger L, et al. Cephalosporin Use in Treatment of Patients with Penicillin Allergies. J Am Pharm Assoc. 2008;48:530-540.
- Goodman EJ, Morgan MJ, Johnson PA, Nichols BA, Denk N, Gold BB. Cephalosporins can be Given to Penicillin-Allergic Patients Who Do Not Exhibit an Anaphylactic Response. J Clin Anesth. 2001;13(8):561-564.
- Mayorga C, Obispo T, Jimeno L, et al. Epitope Mapping of Beta-Lactam Antibiotics with the Use of Monoclonal Antibodies. Toxicology. 1995;97:225-234.
- Nagakura N, Souma S, Shimizu T, Yanagihara Y. Anti-Ampicillin Monoclonal Antibodies and their Cross- Reactivities to Various Beta-Lactams. Br J Hosp Med. 1990;44:252-258.
- Romano A, Viola M, Gueant-Rodriguez RM, Gaeta F, Pettinato R, Gueant JL. Imipenem in Patients with Immediate Hypersensitivity to Penicillins. N Engl J Med. 2006;354:2835-2837.
- Romano A, Viola M, Gueant-Rodriguez RM, Gaeta F, Valluzzi R, Gueant JL. Brief Communication: Tolerability of Meropenem in Patients with IgE-Mediated Hypersensitivity to Penicillins. Ann Intern Med. 2007;146:266-269.
- Shenoy ES, Macy E, Rowe T, Blumenthal KG. Evaluation and Management of Penicillin Allergy: A Review. JAMA. 2019;321(2):188-199.
- Sánchez de Vicente J, Gamboa P, García-Lirio E, Irazabal B, Jáuregui I, Martínez MD, Segurola A, Seras Y, Galán C. Tolerance to Cephalosporins and Carbapenems in Penicillin-Allergic Patients. J Investig Allergol Clin Immunol. 2020;30(1):75-76. doi: 10.18176/jiaci.0463. Epub 2019 Nov 4. PMID: 31680067.
- Romano A, Valluzzi RL, Caruso C, Maggioletti M, Quaratino D, Gaeta F. Cross-Reactivity and Tolerability of Cephalosporins in Patients with IgE-Mediated Hypersensitivity to Penicillins. J Allergy Clin Immunol Pract. 2018 Sep-Oct;6(5):1662-1672. doi: 10.1016/j.jaip.2018.01.020. Epub 2018 Feb 3. PMID: 29408440.
Corticosteroids in Sepsis by Marissa Marks, PharmD
Introduction
- Sepsis is a systemic inflammatory response (SIRS) with associated organ dysfunction as a result of an infection.
- Sepsis is defined as ≥2 of the criteria:
- Temperature >38 ºC or <36 ºC
- Heart rate of >90 bpm
- Respiratory rate of >20 breaths/minute or pCO2 of <32 mmHg
- WBC >12,000 cells/mL or <4000 cells/mL
- Initial management of sepsis includes:
- Intravenous fluids (LR/NS) 30 mL/kg (based on total body weight) administered within the first 3 hours.
- Empiric antibiotic therapy based on the common bacteria and site of infection initiated within the first hour.
- Per the Surviving Sepsis guidelines, IV hydrocortisone is recommended for patients at least 4 hours after initiation of norepinephrine/epinephrine ≥0.25 mcg/kg/min to maintain a MAP of ≥65 mmHg.
Pharmacology
| Hydrocortisone | Methylprednisolone | Fludrocortisone | |
| Dose | IV: 50 mg Q6H or 100 mg Q8H x 5-7 days | IV (succinate): 40 to 125 mg/day (maximum of 1 to 2 mg/kg/day) | PO (in addition to another glucocorticoid): 0.05 mg/day x 7 days |
| Administration | IV: over ≥30 seconds | IV: over several minutes or over 15 to 60 minutes as an infusion | Administer by NG tube |
| PK/PD | -Onset of action (IV): 1 hour -T ½ elimination (IV): 2 +/- 0.3 hours | -Onset of action (IV): 1 hour -T ½ elimination (IV): 0.25 +/- 0.1 hour | -Onset of action (PO): 1-2 hours -T ½ elimination (PO): ~3.5 hours |
| Mechanism of Action | -Anti-inflammatory (decreased synthesis and release of inflammatory mediators) -Immunosuppressive (decreased response to hypersensitivity reactions) -Antiproliferative: vasoconstriction and decreased permeability of WBC to the injury | -Same mechanism of action as hydrocortisone with a 4-5x greater potency | – Mineralocorticoid activity > hydrocortisone or methylprednisolone |
| Adverse Effects | -Cardiovascular: increased blood pressure -Endocrine: fluid retention, hyperglycemia, weight gain -Gastrointestinal: increased appetite -Psychiatric: altered behavior | -Similar adverse effects as hydrocortisone | -Higher risk of fluid retention, hypertension, and decreased electrolyte concentrations |
| Drug Interactions and warnings | –Warnings: adrenal suppression, immunosuppression (higher doses for increased duration of therapy), psychiatric changes -Drug Interactions: antacids (separate by 2 hours), live vaccinations, DDAVP (risk of hyponatremia), succinylcholine | -Warnings: adrenal suppression, acute hepatitis (rare) -Drug Interactions: similar to hydrocortisone and fludrocortisone | -Warnings: patients with underlying hepatic dysfunction, myasthenia gravis, systemic sclerosis, or thyroid disease -Drug Interactions: similar to hydrocortisone and methylprednisolone |
| Compatibility | Drug in Solution: None tested | Drug in Solution: -Compatible: D5W- ½ NS, NS -Incompatible: D5W, D5NS, LR | N/A |
Overview of Evidence
| Author, year | Design/ sample size | Intervention & Comparison | Outcome | |
| French Trial Annane D, 2002. | RCT (n = 300) | hydrocortisone (50-mg intravenous bolus every 6 hours) and fludrocortisone (50- micro g tablet once daily) (n = 151) or matching placebos (n = 149) for 7 days. | 7-day treatment with low doses of hydrocortisone and fludrocortisone significantly reduced the risk of death in patients with septic shock and relative adrenal insufficiency without increasing adverse events. | |
| Teng-Jen Yu, 2009. | RCT (n = 40) | Hydrocortisone 50 mg IV Q6H or methylprednisolone 20 mg Q12H x 7 days | -Higher survival rates with hydrocortisone vs methylprednisolone | |
| VANISH Gordan, 2016 | RCT (n = 1400) | Vasopressin vs. norepinephrine plus hydrocortisone vs. placebo | No significant difference in mortality at 28 days, but vasopressin plus hydrocortisone was associated with faster reversal of shock and reduced need for renal replacement therapy | |
| Gibbison B, 2017. | Systematic review & meta-analysis (n = 33 clinical trials) | Systemic treatment with any corticosteroids | -Decreased septic shock reversal with methylprednisolone vs hydrocortisone -Increased 28-day mortality with methylprednisolone vs dexamethasone -Decreased risk of superinfections with methylprednisolone –Decreased ICU mortality and LOS with methylprednisolone | |
| CORTICUS Sprung, 2018 | RCT, (n=499) | Hydrocortisone 50 mg every 6 hours vs. placebo | The study found no significant difference between the two groups in 28-day mortality, but hydrocortisone was associated with a higher rate of shock reversal and a lower rate of progression to multiple organ dysfunction syndrome. | |
| HYPRESS Key, 2018 | RCT (n = 380) | Infusion of hydrocortisone 200 mg daily for five days followed by tapering until day 11 vs placebo | The study found no significant difference between the two groups in the primary outcome of time alive and free of vasopressor support by day 7 The study also found no significant difference between the two groups in secondary outcomes such as mortality at 28 days, ICU-free days, and hospital-free days | |
| ADRENAL Venkatesh B, 2018. | RCT (n = 3800) | Hydrocortisone 200 mg IV daily | -No difference in 28 or 90-day mortality with hydrocortisone –Decreased time to resolution of septic shock and discharge from the ICU with hydrocortisone -Decreased number of patients received a blood transfusion with hydrocortisone -Higher number of adverse events with hydrocortisone | |
| APROCCHHSAnnane D, 2018. | RCT (n = 1280) | -Hydrocortisone 50 mg IV Q6H + fludrocortisone 50 mcg PO daily in AM x 7 days -Drotrecogin alfa -Combination therapy of the three medications | –Decreased 90-day mortality with hydrocortisone + fludrocortisone -Decreased mortality with hydrocortisone + fludrocortisone at ICU and hospital discharge -Decreased time to discontinue vasopressor therapy and mechanical ventilation and achieve a SOFA score of <6 with hydrocortisone + fludrocortisone | |
Conclusions
- Per the Surviving Sepsis guidelines, hydrocortisone is recommended first-line for the treatment of septic shock in patients that are refractory to fluid (volume) resuscitation.
- Hydrocortisone portrayed greater efficacy in clinical trials than methylprednisolone.
- There are no clinical trials for the comparison of hydrocortisone monotherapy versus hydrocortisone + fludrocortisone; however, it is hypothesized that hydrocortisone provides sufficient mineralocorticoid activity as monotherapy without the increased risks of adverse effects with the addition of fludrocortisone.
- Necessary to avoid fludrocortisone in specific patient populations (i.e. congestive heart failure, hepatic and renal disease, etc.)
References
- Annane D, Buisson CB, Cariou A, Martin C, Misset B, Renault A, Lehmann B, Millul V, Maxime V, Bellissant E; APROCCHSS Investigators for the TRIGGERSEP Network. Design and conduct of the activated protein C and corticosteroids for human septic shock (APROCCHSS) trial. Ann Intensive Care. 2016 Dec;6(1):43.
- Annane D, Renault A, Brun-Buisson C, Megarbane B, Quenot JP, Siami S, Cariou A, Forceville X, Schwebel C, Martin C, Timsit JF, Misset B, Ali Benali M, Colin G, Souweine B, Asehnoune K, Mercier E, Chimot L, Charpentier C, François B, Boulain T, Petitpas F, Constantin JM, Dhonneur G, Baudin F, Combes A, Bohé J, Loriferne JF, Amathieu R, Cook F, Slama M, Leroy O, Capellier G, Dargent A, Hissem T, Maxime V, Bellissant E; CRICS-TRIGGERSEP Network. Hydrocortisone plus Fludrocortisone for Adults with Septic Shock. N Engl J Med. 2018 Mar 1;378(9):809-818.
- Evans L, Rhodes A, Alhazzani W, et al. Surviving sepsis campaign: international guidelines for management of sepsis and septic shock 2021. Intensive Care Med. 2021 Nov;47(11):1181-1247.
- Gibbison B, López-López JA, Higgins JP, Miller T, Angelini GD, Lightman SL, Annane D. Corticosteroids in septic shock: a systematic review and network meta-analysis. Crit Care. 2017 Mar 28;21(1):78.
- Hotchkiss RS, Moldawer LL, Opal SM, Reinhart K, Turnbull IR, Vincent JL. Sepsis and septic shock. Nat Rev Dis Primers. 2016 Jun 30;2:16045.
- Hydrocortisone (2023) UpToDate. Available at: https://www.uptodate.com (Accessed: 13 August 2023).
- Hydrocortisone Sodium Succinate (2023) Micromedex. Available at: https://www.micromedexsolutions.com (Accessed: 13 August 2023).
- Venkatesh B, Finfer S, Cohen J, Rajbhandari D, Arabi Y, Bellomo R, Billot L, Correa M, Glass P, Harward M, Joyce C, Li Q, McArthur C, Perner A, Rhodes A, Thompson K, Webb S, Myburgh J; ADRENAL Trial Investigators and the Australian–New Zealand Intensive Care Society Clinical Trials Group. Adjunctive Glucocorticoid Therapy in Patients with Septic Shock. N Engl J Med. 2018 Mar 1;378(9):797-808.
- Yu TJ, Liu YC, Yu CC, Tseng JC, Hua CC, Wu HP. Comparing hydrocortisone and methylprednisolone in patients with septic shock. Adv Ther. 2009 Jul;26(7):728-35.
- Keh D, Trips E, Marx G, Wirtz SP, Abduljawwad E, Bercker S, Bogatsch H, Briegel J, Engel C, Gerlach H, Goldmann A, Kuhn SO, Hüter L, Meier-Hellmann A, Nierhaus A, Kluge S, Lehmke J, Loeffler M, Oppert M, Resener K, Schädler D, Schuerholz T, Simon P, Weiler N, Weyland A, Reinhart K, Brunkhorst FM; SepNet–Critical Care Trials Group. Effect of Hydrocortisone on Development of Shock Among Patients With Severe Sepsis: The HYPRESS Randomized Clinical Trial. JAMA. 2016 Nov 1;316(17):1775-1785. doi: 10.1001/jama.2016.14799. PMID: 27695824.
- Sprung CL, Annane D, Keh D, Moreno R, Singer M, Freivogel K, Weiss YG, Benbenishty J, Kalenka A, Forst H, Laterre PF, Reinhart K, Cuthbertson BH, Payen D, Briegel J; CORTICUS Study Group. Hydrocortisone therapy for patients with septic shock. N Engl J Med. 2008 Jan 10;358(2):111-24. doi: 10.1056/NEJMoa071366. PMID: 18184957.
- Gordon AC, Mason AJ, Thirunavukkarasu N, Perkins GD, Cecconi M, Cepkova M, Pogson DG, Aya HD, Anjum A, Frazier GJ, Santhakumaran S, Ashby D, Brett SJ; VANISH Investigators. Effect of Early Vasopressin vs Norepinephrine on Kidney Failure in Patients With Septic Shock: The VANISH Randomized Clinical Trial. JAMA. 2016 Aug 2;316(5):509-18. doi: 10.1001/jama.2016.10485. PMID: 27483065.
Ketamine for Treatment of Acute Agitation
Introduction
- Ketamine is a sedative used for patients with extreme/refractory undifferentiated agitation
- Indications for utilizing ketamine for emergent sedation of agitated patients include
- Patient poses and immediate threat to patient and healthcare provider safety (RASS +4)
- Failure and/or futility of alternative non-pharmacologic de-escalation strategies
- Absence of IV access
- Not a candidate for intramuscular antipsychotics and/or benzodiazepines due to onset of action
Pharmacology
| Properties | Rapid acting general anesthetic producing cataleptic-like state due to antagonism of N-methyl-Daspartate (NMDA) receptors in the central nervous system. • Ketamine also has significant analgesic/dissociative properties at lower doses |
| Dose | 2-5 mg/kg IM to a max single dose of 500mg 1-2 mg/kg IV |
| Administration | IM: Inject deep IM into large muscle (glute or vastus lateralis muscle) IV: Administer over at least 60 seconds |
| Formulation | 10 mg/mL, 50 mg/mL, 100 mg/mL *must use 100 mg/mL for IM administration to reduce volume |
| PK/PD (for amnestic effects) | Onset: 3-5 mins IM; <1 minutes IV Duration: 15-25 mins IM; 5-10 minutes IV Bioavailability: 93% IM Metabolism: Extensively through hematic N-demethylation Elimination: Greater than 90% urine, <5% feces |
| Adverse Effects | Hypertension Tachycardia Hypersalivation Nausea and vomiting Laryngospasm Emergence phenomenon during recovery phase Increased muscle function (hyperactivity, twitching, rigidity) |
| Contraindications | • Significant hypertension may be hazardous, ACS, ADHF, and unstable dysrhythmia |
| Warnings and Considerations | Rapid IV administration may increase risk of respiratory depression/apnea Verify concentration of formulation Caution in diagnosed schizophrenia Hypotension in catecholamine depleted states Pregnancy and lactation (crosses placenta) |
Overview of Evidence
| Author, year | Design (sample size) | Intervention & Comparison | Outcome |
| Lin et al., 2020 | Prospective, randomized, pilot (n=93) | Ketamine 4 mg/kg IM or 1 mg/kg IV Haloperidol 5-10 mg IM/IV + lorazepam 1-2 mg IM/IV | Ketamine achieved greater sedation within 5 and 15 minutes (22% vs 0% at 5 mins; 66% vs 7% at 15 mins) |
| Mankowitz et al., 2018 | Systematic review (n=650) | Ketamine IV or IM | Mean time to sedation was 7.21min and effective in 68.5% of patients 30.5% of patients required intubation, but not all secondary to ketamine administration |
| Cole et al., 2016 | Prehospital prospective, observational (n=146) | Haloperidol 10 mg IM Ketamine 5 mg/kg IM | Median time to adequate sedation was faster with ketamine (5 min) vs haloperidol (17 min) • Intubation rates were higher with ketamine (39%) than haloperidol (4%), as well as more complications (49% vs 5%, respectively) 38% hypersalivation in ketamine group |
| Isbister et al., 2016 | Subgroup analysis from DORM II study; prospective, observational (n=49) | Ketamine as rescue treatment after Droperidol alone Droperidol + DZP or MDZ Midazolam alone | Median time to sedation post-ketamine was 20 minutes (IQR 10-30) 3 patients had adverse reactions after ketamine (vomiting n=2; desaturation n=1) |
| Riddell et al., 2016 | Prospective, observational (n=106) | Ketamine Lorazepam, midazolam, haloperidol, or benzodiazepine + haloperidol | Ketamine resulted in a greater number of patients with no agitation at 5 minutes than other medications |
| Scheppke et al., 2014 | Retrospective chart review (n=52) | Ketamine ~4mg/kg IM *Recommended midazolam 2-2.5 mg IM or IV following ketamine for emergence reaction | 96% of patients obtained sedation, mean time to sedation was 2 minutes 3 patients experienced significant respiratory depression About ½ of patients received midazolam |
Trials in Progress
| Barbic et al., Completed March 2020, results pending | Parallel, prospective, randomized, controlled | Ketamine 5mg/kg IM Midazolam 5mg IM + haloperidol 5mg IM | Primary: Time to adequate sedation Secondary: safety and tolerability, requirement of rescue medication |
Conclusions
- Ketamine has been shown to be effective with a quick time to sedation but is not without risks, including respiratory depression
- Used ketamine with caution in patients who have an underlying psychiatric disorder
- Ketamine should be reserved for specific patient populations and as last line for patient/provider safety
References
- Ketamine. Micromedex [Electronic version].
- Barbic D, et al. Trials. 2018;19(1):651. Published 2018 Nov 26.
- Lin M, et al. Am J Emerg Med. 2020. https://doi.org/10.1016/doi:10.1186/s13063-018-2992-x j.ajem.2020.04.013.
- Mankowitz WL, et al. J Emerg Med. 2018;55(5):670-81.
- Cole JB, et al. Clin Toxicol (Phila). 2016;54(7):556–562.
- Isbister GK, et al. Ann Emerg Med. 2016;67(5):581–587.
- Riddell J, et al. Am J Emerg Med. 2017. http://dx.doi.org/10.1016/j.ajem.2017.02.026
- Scheppke KA, et al. WestJEM. 2014;15(7);736-41.
PPIs for the Management of Upper GI Bleed
Introduction
- Upper GI bleed (UGIB) is a common reason for ED visits with a major cause of morbidity, mortality and medical care costs.
- Peptic ulcer accounts for at least 50% of UGIB cases.
- Patients with UGIB usually present with hematemesis, melena and/or hematochezia.
- Upon presentation, hemodynamic status should be evaluated and resuscitation provided if necessary. Resuscitation can include blood transfusion for target hemoglobin of ≥7 g/dl.
- Patients can be risk stratified to low or high-risk using the Rockall score (range 0-7) and Blatchford score (range 0-23).
- Proton pump inhibitors (PPIs) remain one of the mainstays of pharmacological therapy for the management of UGIB. It can be initiated if endoscopy cannot be performed, will be delayed for >24 after presentation or following endoscopy.
| Pantoprazole | Esomeprazole | Omeprazole | |
| Dose | Initial Infusion: 80mg bolus then 8mg/hr continuous infusion for a total of 72hours Intermittent: 80mg LD then 40mg IVP Q12H Maintenance High-risk: 40mg PO BID for 14days, then 40mg PO once daily Low-risk: 20mg PO once daily *Duration ranges from 4-12weeks | Initial Infusion: 80mg bolus then 8mg/hr continuous infusion for a total of 72hours Intermittent: 80mg LD then 40mg IVP Q12H Maintenance High-risk: 40mg PO BID for 14days, then 40mg PO once daily Low-risk: 20mg PO once daily *Duration ranges from 4-12weeks | Initial IV Omeprazole not available in the U.S, give IV Pantoprazole or Esomeprazole Maintenance High-risk: 40mg PO BID for 14days, then 40mg PO once daily Low-risk: 20mg PO once daily *Duration ranges from 4-12weeks |
| Administration | IVP: Give over at least 2 minutes Continuous Infusion: 8mg/hr PO: Swallow whole without crushing or splitting 30-60minutes before food | IVP: Give over at least 3 minutes for dose <80 mg; Loading dose over 30 minutes Continuous Infusion: 8mg/hr PO: Capsule can be given orally or opened and mixed with 50mL water for NG administration | PO: Swallow whole without crushing or splitting 30-60minutes before food |
| PK/PD | Onset: IV 15 to 30 minutes, PO 2.5hrs Absorption: Rapid, well absorbed Duration: 24hours (IV and PO) Distribution: 98% albumin bound Half-life elimination: 1hr, 3.5-10hrs in CYP2C19 deficiency Excretion: Urine (71%), feces (18%) | Distribution: 97% protein bound Metabolism: Hepatic primarily via CYP2C19 Half-life elimination: 1 to 1.5hrs in adults Excretion: Urine (80%), 20% feces | Onset: PO 1hr Absorption: Rapid Duration: Up to 72hours Distribution: 95% albumin bound Half-life elimination: 30min – 1hr, 3 hrs in hepatic impairment Excretion: Urine (77%) |
| Adverse Effects | Headache, nausea, abdominal pain, diarrhea, vomiting | Headache, flatulence, nausea, dyspepsia, abdominal pain, diarrhea | Headache, abdominal pain, nausea, diarrhea, vomiting, flatulence |
| Drug Interactions & Warnings | Contraindicated with Atazanavir, Rilpivirine and their combinations | Contraindicated with Atazanavir, Rilpivirine and their combinations, CYP2C19 Inducers | Contraindicated with Atazanavir, Rilpivirine and their combinations, CYP2C19 Inducers |
| Compatibility | Compatible with D5W, NS or LR | Compatible with D5W, NS or LR | Not Applicable |
Overview of Evidence
| Author, year | Design & Sample Size | Intervention & Comparison | Outcomes |
| Daneshmend et al., 1992 | Double-blind, placebo- controlled, parallel study (n=1147) | Omeprazole 80mg IV bolus followed by 40mg IV every 8hr x3, then 40mg PO twice daily vs placebo Treatment started within 12h of admission, continued for 4 days or until surgery, discharge or death | No significant differences between placebo and omeprazole for blood transfusions (53% v 52%), rebleeding (18% v 15%), surgery (11% v 11%) and death (5.3% v 6.9%) Significant reduction in signs of UGIB observed during endoscopy with omeprazole (33%) vs placebo (45%); p < 0.0001 |
| Andriulli et al., 2008 | Randomized, multicenter double-blind study (n=474) | PPI Continuous (80mg bolus followed by 8mg/hr infusion for 72hr) PPI Intermittent (40mg IV bolus daily for 72hr) Switched to oral PPI (20 mg twice daily) after 72hr and continued until discharge Used Pantoprazole and Omeprazole | Bleeding recurred in 11.8% continuous regimen vs 8.1% in the intermittent regimen; P = 0.18 7.6% vs 8.1% rebleeding during first 72hr in the continuous vs intermittent group; P = 0.32 Patients in the continuous group had a prolonged hospital stay > 5 days (P = 0.03) |
| Sung et al., 2009 | Randomized, multicenter double-blind study (n=764) | Esomeprazole 80mg IV bolus followed by 8mg/hr Placebo, continued for 72hr after endoscopic hemostasis o Both groups received esomeprazole PO 40mg daily for 27days after infusion | Esomeprazole had less recurrent bleeding within 72hr compared to placebo (5.9% vs 10.3%). Findings remained significant at day 7 and day 30; p = 0.010 Esomeprazole decreased endoscopic re-treatment (6.4% vs 11.6%), need for surgery (2.7% vs 5.4%) and mortality (0.8% vs 2.1%) |
| Sreedharan et al., 2010 | Systematic review and meta-analysis (6RCTs, n=2223) | Active treatment with a PPI (oral or IV) and control with either placebo, histamine-2 receptor antagonist or no treatment before endoscopy | PPI before endoscopy did not decrease mortality (OR 1.12 95% CI 0.72-1.73), rebleeding (OR 0.81, 95% CI 0.61- 1.09) or the need for surgery (OR 0.96, 95% CI 0.68-1.35) PPIs significantly decreased the number of patients with stigmata of recent hemorrhage at endoscopy PPIs compared to control significantly reduced endoscopic intervention |
| Chen et al., 2012 | Prospective, randomized control trial (n=201) | Pantoprazole 80mg IV bolus then 8mg/hr Pantoprazole 40mg IV bolus once daily for 72hr o Both groups received pantoprazole 40mg daily PO for 27days after 72hr | No statistical differences in units of blood transfused, length of hospital stay, surgical/radiological interventions and mortality within 30 days High-dose PPI regimen was not superior in the reduction of recurrent bleeding at 30 days as compared with a standard-dose regimen |
| Sachar et al., 2014 | Systematic review and meta-analysis (13RCTs) | Intermittent doses of PPIs (IV or PO) 80mg IV bolus followed by 8mg/hr for 72hours | Intermittent PPI regimens were comparable and are non-inferior to continuous PPI infusion regimens in patients with bleeding ulcers and high-risk endoscopic findings. There is no difference in recurrent bleeding with intermittent vs continuous PPI therapy |
| Rattanasupar et al., 2016 | Prospective, randomized control trial (n=113) | Pantoprazole 80mg IV bolus then 8mg/hr Pantoprazole 40mg IV twice daily | No difference in average time of hospital stay (3.03 vs 2.89 days, p>0.05) and mean amount of blood transfused (1.79 vs 1.63 units, p>0.05) between continuous and intermittent pantoprazole No statistically significant difference in terms of recurrent bleeding and mortality between both groups (p>0.05) Blatchford score greater than 10, 11, and 12 showed high sensitivity of predicting high-risk peptic ulcer bleeding |
Conclusions
- Compared to placebo or other non-PPI treatment measures, evidence suggests PPI therapy did not reduce the need for blood transfusion, rebleeding rate, surgery or death.
- Compared to placebo, PPIs reduced the signs of upper gastrointestinal bleeding observed during endoscopy and reduced the need for endoscopic treatment.
- Administration of a PPI as continuous infusion did not impact patient outcomes and is not superior to intermittent therapy; however, high dose PPI may be considered in patients with Blatchford scores greater than 12.
References
- Clinical Pharmacology [Electronic version]. Elsevier, 302 Knights Run Ave., Suite 800, Tampa, FL 33602. Retrieved February 17, 2021, from http://www.clinicalpharmacology-ip.com/
- Uptodate [Electronic version]. Retrieved February 15, 2021, from http://www.uptodate.com/
- Laine, Loren MD; Jensen, Dennis M MD. Management of Patients With Ulcer Bleeding, American Journal of Gastroenterology: March 2012 – Volume 107 – Issue 3 – p 345-360
- Daneshmend, T. K., Hawkey, C. J., Langman, M. J., Logan, R. F., Long, R. G., & Walt, R. P. (1992). Omeprazole versus placebo for acute upper gastrointestinal bleeding: randomised double blind controlled trial. BMJ (Clinical research ed.), 304(6820), 143–147.
- Andriulli, A., Loperfido, S., Focareta, R., Leo, P., Fornari, F., Garripoli, A., Tonti, P., Peyre, S., Spadaccini, A., Marmo, R., Merla, A., Caroli, A., Forte, G. B., Belmonte, A., Aragona, G., Imperiali, G., Forte, F., Monica, F., Caruso, N., & Perri, F. (2008). High- versus low-dose proton pump inhibitors after endoscopic hemostasis in patients with peptic ulcer bleeding: a multicentre, randomized study. The American journal of gastroenterology, 103(12), 3011–3018.
- Sung JJ, Barkun A, Kuipers EJ, et al. Intravenous esomeprazole for prevention of recurrent peptic ulcer bleeding: a randomized trial. Ann Intern Med. 2009; 150(7):455-464.
- Sreedharan, A., Martin, J., Leontiadis, G. I., Dorward, S., Howden, C. W., Forman, D., & Moayyedi, P. (2010). Proton pump inhibitor treatment initiated prior to endoscopic diagnosis in upper gastrointestinal bleeding. The Cochrane database of systematic reviews, 2010(7), CD005415.
- Chen CC, Lee JY, Fang YJ, et al. Randomised clinical trial: high-dose vs. standard-dose proton pump inhibitors for the prevention of recurrent haemorrhage after combined endoscopic haemostasis of bleeding peptic ulcers. Aliment Pharmacol Ther. 2012; 35(8):894-903.
- Sachar H, Vaidya K, Laine L. Intermittent vs continuous proton pump inhibitor therapy for high-risk bleeding ulcers: a systematic review and meta-analysis. JAMA Intern Med. 2014; 174(11):1755-1762.
- Rattanasupar A, Sengmanee S. Comparison of High Dose and Standard Dose Proton Pump Inhibitor before Endoscopy in Patients with Non-Portal Hypertension Bleeding. J Med Assoc Thai. 2016; 99(9):988-995.
Single-Dose Aminoglycosides for UTIs
Hypertonic Saline Versus Mannitol for ICP Reduction
Introduction
- Elevated intracranial pressure (ICP) is caused by excess volume in the cerebral spaces, which causes a reduction in the cerebral perfusion pressure and affects blood flow and oxygenation to the brain.
- Hyperosmolar agents (hypertonic saline and mannitol) are utilized to form a gradient across the blood-brain barrier to draw fluid from the cerebral space into the vasculature, thus reducing ICP
- Mannitol was previously considered the gold standard of osmotic therapy, but hypertonic saline has proven to be at least as effective as mannitol at reducing ICP
Pharmacology
| Hypertonic Saline | Mannitol | |
| Mechanism | Increases serum sodium levels, making it more hypertonic. Giving a bolus causes a gradient for water to follow sodium extracellularly and move out of the cerebral spaces into the vasculature, while a continuous infusion aids in resuscitation | Osmotic diuretic by increasing the osmolality of the glomerular filtrate, thus blocking reabsorption of water and excretion of sodium. This leads to movement of water to extracellular and vascular spaces and reducing the ICP |
| Dose | 3 – 23.4% available 3%: optimal dose is unclear, reasonable to start with 300-500mL bolus or continuous infusion at 100mL/hr and titrate per response 23.4% : 0.43-0.5 mL/kg IV bolus, max 30mL/dose | 5 – 25% solutions available (20% most common) 0.25 – 1g/kg/dose IV bolus q 6-8 hours (Usually 25-100g per dose) |
| Administration | 3% intermittent bolus or continuous infusion *strong osmotic gradient not retained with continuous infusions 23.4% intermittent bolus over 15 minutes | Intermittent IV infusion over 30 minutes |
| Adverse Effects | Hypervolemia, respiratory distress, electrolyte imbalances (hypernatremia) | Hypotension, hypovolemia, AKI, electrolyte disturbances (specifically K+), extravasation |
| Cautions/Pearls | Solutions > 3-5% require a central line | Requires in-line filter due to risk of crystallization Avoid in hypovolemia and anuria |
| Patient population to consider use in | Hypovolemic, hypotensive, traumatic resuscitation | Euvolemia, hypertensive, fluid restrictions |
| Monitoring | Serum sodium 145-155mEq/dL Serum osmolality 300-320 mOsm/L Titrate based on ICP | Serum osmolality 300-320 mOsm/L Titrated based on ICP |
| Where to find in GHS | 3% Sodium chloride – 500mL EDZONE2, EDZONE3, ALL TRAUMA STATIONS | 20% Mannitol – 500ML EDZONE2, EDZONE3, TRAUMA-M, EDETENTION |
Considerations for Administration
| 3% Sodium Chloride | 23.4% Sodium Chloride | 20% Mannitol | |
| Vascular Access | Peripheral or central | Central ONLY | Peripheral or central |
| Volume (per dose) | 500mL + | ~30 mL | 125 – 500 mL(20%) |
| Equipment | Bolus: Infusion by gravity Continuous: IV infusion pump | Syringe pump preferred | IV infusion pump |
Overview of Evidence
| Author, year | Design/ sample size | Intervention & Comparison | Outcome |
| A. Kerwin, 2009 | Retrospective analysis, (22 patients) | HTS vs mannitol mean ICP reduction in patients with TBI | HTS is as efficacious as mannitol, if not more so, and adds to the growing literature suggesting that HTS is an effective modality for the control of elevated ICP in patients with severe TBI |
| M. Li, 2015 | Meta-Analysis, 7 studies (169 patients) | HTS vs mannitol in mean ICP reduction in patients with TBI | HTS reduces ICP more effectively than mannitol in the setting of TBI |
| S. Burgess, 2016 | Meta-Analysis, 7 trials (191 patients) | HTS vs mannitol in mean ICP reduction, risk of ICP treatment failure, mortality rates, and neurological outcomes | No statistical difference in mortality and neurological outcomes. No difference in mean reduced ICP; decreased risk of ICP treatment failure with HTS |
| E. Berger- Pelleiter, 2016 | Meta-Analysis, 11 studies (1,820 patients) | HTS vs mannitol in reduction of mortality, ICP, and increasing functional outcomes | No significant reduction in mortality, no significant reduction in mean ICP, no significant difference in functional outcomes |
| C. Pasarikovski, 2017 | Systematic Review, 5 studies (175 patients) | HTS vs mannitol in ICP reduction in aneurysmal subarachnoid hemorrhage | No difference between mannitol and 3% HTS in reducing ICP in patients with aneurysmal subarachnoid hemorrhage |
| J. Gu, 2018 | Mata-Analysis, 12 RCTs, (438 patients) | HTS vs mannitol in ICP reduction, ICP control, changes in serum sodium and osmolality, mortality, neurological function outcome | No difference in mean ICP reduction, neurological function, and mortality. HTS may be preferred in TBI patients with refractory intracranial hypertension |
References
- Burgess S, et al. Annals of pharmacotherapy. 2016;50(4):291-300.
- Li M, et al. Y, 2015. Medicine. 2015;9(4):17.
- Dastur C, et al. Stroke and vascular neurology. 2017;2:21-29.
- Kerwin A, et al. J Trauma. 2009;67:277-282.
- Pasarikovski C, et al. World Neurosurg. 2017;105:1-6.
- Gu J, et al. Neurosurg Rev. 2018;42:499.
- Berger-Pelleiter E, et al. CJEM. 2016;18:112–120.
- Farrokh S, et al. Curr opin crit care. 20119; 25:105-109.
- Witherspoon B, et al. Nurs Clin N Am. 2017;52:249-60.
- Micromedex [Electronic].Greenwood Village, CO: Truven Health Analytics. Retrieved August 12, 2019 from http://www.micromedexsolutions.com
10 Things You Can Do If You Don’t Match for a Pharmacy Residency Program
As pharmacy residency application season comes to a close, it’s time to take a deep breath and reflect on the experience. Regardless of the outcome, it’s important to remember that you’ve put in a tremendous amount of effort and dedication to get to this point.
Things didn’t go as planned but here’s 10 things you can do now to try to focus on what you can versus what you cannot.
10 Things to Do
- Do not panic or lose hope. Not matching is not the end of your career and there are still opportunities to pursue your goals
- Review your application materials and identify areas of improvement. Seek feedback from mentors, preceptors, faculty members, or peers who can help you improve your CV, letter of intent, interview skills, etc
- Consider participating in Phase II of the Match or the Post-Match Scramble. Phase II is another round of matching for programs that still have unfilled positions after Phase I. The Post-Match Scramble is an informal process where applicants can contact programs directly after Phase II to inquire about any remaining vacancies
- Be flexible and open-minded about your options. You may need to expand your geographic preferences, consider different types of programs or settings, or apply for non-traditional residencies such as fellowships or industry positions
- Network and stay connected with potential employers, mentors, preceptors, faculty members, alumni, or colleagues who can offer you advice, support, referrals, or opportunities.
- Update your online profiles and portfolios such as LinkedIn, ePortfolio, ASHP Connect etc., to showcase your achievements, skills, and interests.
- Seek out additional learning opportunities such as continuing education courses, certificate programs, webinars, podcasts, journals, etc., to enhance your knowledge and skills and demonstrate your commitment to professional development
- Explore alternative career paths or transitional roles that can help you gain valuable experience and exposure to different aspects of pharmacy practice such as clinical pharmacist, staff pharmacist, adjunct faculty member, consultant pharmacist, etc
- Maintain a positive attitude and a growth mindset. Do not let rejection or failure define you or discourage you from pursuing your goals. Learn from your mistakes and challenges and use them as opportunities to improve yourself
- Seek professional help or support if needed. Not matching can be a stressful and emotional experience that can affect your mental health and well-being. Do not hesitate to reach out to counselors, therapists, coaches, mentors, friends, family members, or other sources of support who can help you cope with your feelings and provide you with guidance and encouragement.
Good Luck with the next phase of your life
Beyond Residency Applications: How to Focus on Self-Improvement and Growth
As pharmacy residency application season comes to a close, it’s time to take a deep breath and reflect on the experience. Regardless of the outcome, it’s important to remember that you’ve put in a tremendous amount of effort and dedication to get to this point. Now, it’s time to shift your focus to other areas of your life.
One of the most important things you can do during this time is to focus on yourself. This means taking the time to catch up on any projects, research, or top discussions that were put on hold due to residency application season. It also means making time for things outside of pharmacy, such as exercising, reading, or even binge-watching a new Netflix series.
By focusing on something outside of pharmacy, you can clear your mind and approach your work with a fresh perspective. People who are flexible, open-minded, and hard-working will make the best out of every situation and get more from a residency program than other candidates simply due to the fact that they have an open mindset compared to having a fixed mindset.
Residency training has gotten larger and more structured, which means that there will be a great program for you no matter where you end up. Trust that you got it right with your rank list, and that you will end up in the best scenario. Be open to learning and growing, and you will make the most out of your residency program.
And if you don’t match, that’s okay too. There are other routes you can take to get to the ultimate goal of using your pharmacy degree to the maximum and getting the job you desire. Don’t be discouraged – keep pushing forward and pursuing your dreams.
Remember, it’s important to take care of yourself and your well-being during this time. If you have any thoughts or comments, please feel free to share them with us in the comments section below. We’d love to hear from you.
Management of Hypertensive Emergency
Introduction
- Hypertensive emergency is characterized by systolic blood pressure (SBP) > 180 mmHg or diastolic blood pressure (DBP) > 120 mmHg with evidence of target organ damage.
- Rapid blood pressure lowering with intravenous antihypertensives is warranted to prevent further organ damage.
- Patients presenting with intracranial hemorrhage, aortic dissection, preeclampsia, or pheochromocytoma crisis should achieve target blood pressure within one hour of presentation.
- Current literature lacks evidence of mortality benefit with any one antihypertensive drug. Selection of a medication should consider target organ(s) affected, underlying disease states, and time to target blood pressure.
Treatment in Selected Co-Morbidities
| Condition | BP Goal | Preferred Agents |
| Acute aortic dissection | SBP < 120 mmHg within 20 min | Esmolol Labetalol Nicardipine Nitroprusside |
| Eclampsia or Preeclampsia | SBP < 140 mmHg within 1 hour | Nicardipine Labetalol Hydralazine |
| Pheochromocytoma (catecholamine excess) | SBP < 140 mmHg within 1 hour | Nicardipine Phentolamine* |
| Intracranial hemorrhage | SBP < 160 mmHg within 6 hours | Nicardipine Labetalol |
| Acute ischemic stroke | Pre-alteplase: < 185/110 mmHg Post-alteplase: < 180/105 for 24 hours No thrombolytic: SBP reduced 15% in 24 hours** | Nicardipine Labetalol |
**Permissive hypertension may be reasonable; maintain SBP < 220 mmHg or DBP < 120 mmHg
Pharmacology: Intravenous Antihypertensives
| First-line Agents | |||||
| Medication | Class | Onset | Duration | Dosing | Clinical Pearls |
| Nicardipine | Ca channel blocker | IV: 5-10 min | IV: 2-6 hours | Initial: 5 mg/hr Titration: 2.5 mg/hr every 15 min Maximum: 15 mg/hr | No dose adjustments in elderly patients |
| Esmolol | Beta-blocker | IV: 1-2 min | IV: 10-20 min | Bolus: 500-1,000 mcg/kg Initial: 50 mcg/kg/min Titration: repeat bolus dose, then increase by 50 mcg/kg/ min every 10 min Maximum: 200 mcg/kg/min | Contraindications: Bradycardia Decompensated HF |
| Labetalol | Beta-blocker Alpha-1 antagonist | IV: 2-5 min Peak: 5-15 min | IV: 2-6 hours Peak: 18 hours | Bolus: 10-20 mg IV push every 10 min IV infusion: 0.5 – 10 mg/min titrated 1-2 mg/min every 2 hours Maximum: 300 mg total | Precaution: Second-/thirddegree heart block Bradycardia Heart failure |
| Second-line Agents | |||||
| Phentolamine* | Non-selective alpha antagonist | IV: Seconds | IV: 15 min | Initial: 5 mg IV push May repeat every 10 min PRN | Useful in catecholamine excess and clonidine withdrawal |
| Nitroglycerin | NOdependent vasodilator | IV: 2-5 min | IV: 5-10 min | ACS: Initial: 5 mcg/min Titration: 5 mcg/ min every 3-5 min Maximum: 20 mcg/min Pulmonary edema: Initial: 100-200 mcg/min Titration: 50 mcg/min every 3-5 min Maximum: 400 mcg/min | Indicated in ACS or pulmonary edema Use caution in volume-depleted patients |
| Sodium nitroprusside | NOdependent vasodilator | IV: Seconds | IV: 1-2 min | Initial: 0.3-0.5 mcg/kg/min Titration: 0.5 mcg/kg/min every 1 min Maximum: 10 mcg/kg/min | Requires intra-arterial BP monitoring Tachyphylaxis and cyanide toxicity with prolonged use – Limit treatment duration |
| Hydralazine | Direct vasodilator | IV: 10 min IM: 20 min | IV: 1-4 hours IM: 2-6 hours | Initial: 10-20 mg IV push Repeat every 4-6 hours PRN | Not available as an IV infusion |
| Enalaprilat | ACE inhibitor | IV: 15-30 min | IV: 12-24 hours | Initial: 1.25 mg IV over 5 min Titration: increase by 5 mg every 6 hours as needed | Slow onset (~15 min) Contraindications: Pregnancy MI Bilateral renal stenosis |
Overview of Evidence
| Author (Title), Year | Design | Purpose | Outcome |
| Anderson (INTERACT), 2008 | RCT (N=404) | Comparison of BP goals (SBP < 140 vs SBP < 180) in patients with acute ICH | Mean hematoma expansion was smaller in the intensive group (13.7% vs 36.3%) No difference in death or disability at 3 months (48% vs 49%) Limitation: included patients with SBP > 150 mmHg, over 30% of patients were treated with oral antihypertensive therapy |
| Quereshi (ATACH-2), 2016 | RCT (N=1,000) | Comparison of BP goals (SBP 110-139 vs SBP 179-140) in patients with acute ICH | All patients received nicardipine infusion No difference between death or disability at 3 months (38.7% vs 37.7%) Increased renal adverse events within 24 hours in the intensive group (9.0% vs 4.0%) Limitation: mean SBP differed by only 10 mmHg between groups 2 hours post-randomization (129 mmHg vs 141 mmHg) |
| Peacock (CLUE), 2011 | RCT (N=226) | Nicardipine IV infusion versus labetalol IV bolus for management of hypertensive emergency | Patients receiving nicardipine were more likely to reach target BP within 30 min (91.7% vs 82.5%) Rescue antihypertensive use did not differ significantly between groups within first 6 hours Limitation: only 63.3% of patients had evidence of target organ damage at randomization |
| Yang, 2004 | Prospective cohort (N=40) | Nitroprusside IV versus nicardipine IV for hypertensive emergency with pulmonary edema | No significant difference between blood pressure readings across groups at any time point No adverse events reported in either group Limitation: nicardipine dosing started at 3 mcg/kg/min (12.5 mg/hr in a 70 kg patient) |
Conclusions
- Selection of a first-line antihypertensive should consider compelling indications and acute blood pressure goals, as robust literature comparing long-term outcomes across drug classes is lacking for most indications.
- Nicardipine may provide more consistent blood pressure control than labetalol. This is particularly important in patients with acute stroke, as large fluctuations in blood pressure are believed to negatively impact cerebral perfusion.
- Aggressive lowering of SBP less than 140 mmHg in patients with acute ICH has not been shown to improve long-term outcomes and may negatively impact renal perfusion.
- Nicardipine has been shown to provide similar blood pressure control to nitroprusside. In patients with acute ICH, nitroprusside use within 24-hours of presentation was associated with higher in-hospital mortality.
References
- Whelton, et al. 2017 ACC/AHA/AAPA/ABC/ACPM/AGS/APhA/ASH/ASPC/NMA/PCNA Guideline for the Prevention, Detection, Evaluation, and Management of High Blood Pressure in Adults. J Amer Heart Assoc 2018;71(6):e13-e115.
- Benken ST. Hypertensive emergencies. CCSAP 2018;1:7-30.
- Anderson, et al. Intensive blood pressure reduction in acute cerebral haemorrhage trial (INTERACT): a randomised pilot trial. Lancet Neurol 2008;7:391-9.
- Quereshi, et al. Intensive blood-pressure lowering in patients with acute cerebral hemorrhage. New Engl J Med 2016;375(11):1033-43.
- Peacock WF, et al. CLUE: a randomized comparative effectiveness trial of IV nicardipine versus labetalol use in the emergency department. Critical Care 2011;15(R157):1-8.
- Yang HJ, Kim JG, Lim YS, et al. Nicardipine versus nitroprusside infusion as antihypertensive therapy in hypertensive emergencies. J Int Med Res 2004;32:118-23.
Fibrinolytics for STEMI
Introduction
- Percutaneous coronary intervention (PCI) is the preferred reperfusion strategy during a cardiac arrest; thrombolytic therapy is an option without PCI capability, followed by transfer to a PCI capable center.
- Thrombolytic therapy is most effective when administered within 30 minutes of first medical contact, however, may be considered within 12 – 24 hours of symptom onset and ongoing ischemia or extensive ST elevation.
- During ACS-Induced Cardiac Arrest, the goal for fibrinolysis is 30 minutes and reperfusion with PCI is preferred, however, if PCI is delayed, fibrinolytics therapy could be considered.
Pharmacology
| Alteplase | Tenecteplase | |
| MOA | Initiates fibrinolysis by binding to fibrin in a thrombus and converts entrapped plasminogen to plasmin | Promotes initiation of fibrinolysis by binding to fibrin and converting plasminogen to plasmin; similar to alteplase but more fibrin specific |
| Dose | Weight based: > 67kg: infuse 15mg IV bolus over 1-2 minute, followed by 50mg infusion over 30 minutes, then 35mg over 1 hour (max total dose 100mg) ≤ 67kg: : infuse 15mg IV bolus over 1-2 minutes, followed by 0.75mg/kg infusion over 30 minutes, then 0.5mg/kg over 1 hour (max total dose 100mg) | Weight based: < 60kg: 30mg ≥ 60 to < 70kg: 35mg ≥ 70 to < 80kg: 40mg ≥ 80 to < 90kg: 45mg ≥ 90kg: 50mg |
| Administration | • Bolus administered over 1 minute followed by infusion | • Single bolus over 5 seconds |
| PK/PD | Duration: 1 hour after infusion terminated Distribution: approximates plasma volume Half-life elimination: 5 minutes Excretion: hepatic and plasma clearance | Distribution: weight related Metabolism: hepatic Half-life elimination: biphasic; initial 20-24 min, terminal 90-130 min Excretion: plasma clearance |
| Adverse Effects | Intracranial hemorrhage Ecchymosis GI/GU hemorrhage Sepsis Cerebrovascular accident | Hemorrhage and hematoma Cerebrovascular accident |
| Drug Interactions and Warnings | Tranexamic acid, avoid combination Internal bleeding, thromboembolic events, cholesterol embolization | Tranexamic acid, avoid combination Internal bleeding, thromboembolic events, arrhythmias |
| Contraindications | Active internal bleeding Ischemic stroke within 3 months except when within 4.5 hours Severe uncontrolled hypertension | Active internal bleeding Severe uncontrolled hypertension Recent intracranial/intraspinal surgery Ischemic stroke within 3 months |
| Compatibility | May be diluted in equal volume with: 0.9% sodium chloride D5W | • Incompatible with dextrose |
Overview of Evidence
| Author, year | Design/ sample size | Intervention & Comparison | Outcome |
| Guillermin 2016a | Meta-analysis of RCT (n=18,208) | • Tenecteplase 30-50mg vs alteplase 80-100mg | Bleeding 4.8% in tenecteplase vs 5.8% alteplase (p=0.0002) No difference in mortality at 30 days |
| Llevadot 2001 | Retrospective review (38 studies) | Reteplase Anoteplase Tenecteplase | Tenecteplase and reteplase associated with accelerated infusion and more convenient by bolus administration Administration of a less fibrin-specific agent may cause greater systemic coagulopathy with potential for more bleeding |
| Boersma 1996 | Retrospective review (n=50,246) | • Fibrinolytic therapy vs placebo | • Mortality reduction in patients treated within 2 hours compared to later (p=0.001) |
| GUSTO 1993 | Randomized, controlled trial (n=41,021) | Streptokinase + SQ heparin Streptokinase + IV heparin Alteplase + IV heparin Alteplase + Streptokinase + IV heparin | Atleplase administered over 1.5 hours with IV heparin provide survival over standard therapy Thrombolytic therapy administered within 2448 hours of admission |
| Armstrong 2013b | Randomized controlled trial (n=1892) | • PCI vs bolus tenecteplase, clopidogrel, and enoxaparin | Tenecteplase administration prehospital resulted in effective reperfusion when PCI was not completed within 1 hour Fibrinolytic therapy associated with increase risk of intracranial bleeding |
| Cardiac Arrest Data | |||
| Bottiger 2001 | Prospective cohort (n=40) | • Alteplase 50 mg bolus, repeat 50 mg in 30 minutes vs placebo | • Increase in ROSC (68% vs 44%), ICU admission compared to placebo |
| Schreiber 2002 | Retrospective chart review (n=157) | • Alteplase 15mg bolus followed by 50mg infusion over 30 min and 35mg over 60 min | • Thrombolytic therapy achieved better functional neurological recovery more frequently (p=0.03) |
| Lederer 2004 | Retrospective chart review (n=108) | • Alteplase 100 mg (15 mg followed by 85 mg over 90 min) | 81% of patients who received thrombolytic therapy were discharged without neurological deficit 67% of patients were still alive 5-10 years after the event |
| Li 2006 | Meta-analysis | • Alteplase 15mg bolus followed by 50mg infusion over 30 min and 35mg over 60 min | Thrombolytic therapy improved the rate of ROSC (p < 0.01) 48% of patients had acute coronary artery obstruction |
| Bottiger 2008 | Randomized, double-blind, multicenter trial (n=1050) | Tenecteplase 30mg if < 60kg Tenecteplase 35mg if 60-69kg • Tenecteplase 40mg if 70-79kg Tenecteplase 45mg if 80-89kg Tenecteplase 50mg if > 90kg Placebo | No difference in tenecteplase and placebo in 30-day survival, ROSC, survival, or neurologic outcomes Increased intracranial hemorrhages in tenecteplase patients |
| RuizBailen 2001 | Retrospective cohort (n=303) | Streptokinase Alteplase accelerated regimen Alteplase double bolus | Systemic thrombolysis patients had a lower mortality, less mechanical ventilation, fewer CPR attempts (p < 0.0001) No fatal hemorrhagic complications |
Conclusions
- Evidence supports PCI is the first line option for management of patients requiring reperfusion during cardiac arrest when a STEMI is suspected
- Available evidence suggests tenecteplase and alteplase are appropriate fibrinolytic therapies when PCI is unavailable
- Tenecteplase is an alternative fibrinolytic therapy and has been evaluated safe and efficacious as a bolus dose of 30-50mg
- When alteplase is the only fibrinolytic therapy available, there is data to support bolus therapy +/- a weight based infusion during cardiac arrest
- Thrombolytic agents administered during CPR can improve the rate of survival but are associated with a risk of severe bleeding
References
- Lexicomp [Electronic version]. Macedonia, OH: Truven Wolters Kluwer Health. Retrieved January 26, 2021, from https://online.lexi.com/lco/action/login.
- Guillermin A, Yan D, Perrier A, Marti C. Safety and efficacy of tenecteplase versus alteplase in acute coronary syndrome: a systematic review and meta-analysis of randomized trials. Arch Med Sci 2016; 12, 6: 1181–1187.
- Llevadot J, Giugliano R, Antman E. Bolus fibrinolytic therapy in acute myocardial infarction. JAMA. 2001; 286(4): 442-449.
- Boersma E, Maas A, Deckers J, Simoons M. Early thrombolytic treatment in acute myocardial infarction: reappraisal of the golden hour. Lancet. 1996; 348: 771-775.
- GUSTO Investigators. An international randomized trial comparing four thrombolytic strategies for acute myocardial infarction. NEJM. 1993; 329(10): 673-682.
- Armstrong P, Gershlick A, Goldstein P, Wilcox R, Danays T, Lambert Y, Sulimov V, Ortiz F, Ostojic M, Welsh R, Carvalho A, Nanas J, Arntz H, Halvorsen S, Huger K, Grajek S, Fresco C, Bluhmki E, Regelin A, Vandenberghe K, Bogaerts K, de Werf F. Fibrinolysis or primary PCI in STSegment elevation myocardial infarction. NEJM. 2013; 268(15):1379-1387.
- Wilcox R. Randomized, double-blind comparison of reteplase double-bolus administration with streptokinase in acute myocardial infarction (INJECT): trial to investigate equivalence. Lancet. 1995; 346(8971):329-336.
- Van de Werf F, Cannon CP, Luyten A, Houbracken K, McCabe CH, Berioli S, Bluhmki E, Sarelin H, Wang-Clow F, Fox NL, Braunwald E. Safety assessment of single-bolus administration of TNK tissue-plasminogen activator in acute myocardial infarction: the ASSENT-1 trial. The ASSENT-1 Investigators. Am Heart J. 1999 May;137(5):786-91. doi: 10.1016/s0002-8703(99)70400-x. PMID: 10220625.
- Lederer W, Lichtenberger C, Pechlaner C, et al. Recombinant tissue plasminogen activator during cardiopulmonary resuscitation in 108 patients with out-of-hospital cardiac arrest. Resuscitation. 2001;50(1):71—76.
- Schreiber W, Gabriel D, Sterz F, et al. Thrombolytic therapy after cardiac arrest and its effect on neurological outcome. Resuscitation. 2002;52(1):63—69.
- Lederer W, Lichtenberger C, Pechlaner C, et al. Longterm survival and neurological outcome of patients who received recombinant tissue plasminogen activator during out-of-hospital cardiac arrest. Resuscitation. 2004;61(2):123—129.
- Li X, Fu QL, Jing XL, et al. A meta-analysis of cardiopulmonary resuscitation with and without the administration of thrombolytic agents. Resuscitation. 2006;70(1):31—36.
- Bottiger BW, Arntz HR, Chamberlain DA, et al. Thrombolysis during resuscitation for out-of-hospital cardiac arrest. NEJM. 2008;359(25):2651—2662.
- Kurkciyan I, Meron G, Sterz F, et al. Major bleeding complications after cardiopulmonary resuscitation: impact of thrombolytic treatment. J Intern Med. 2003;253(2):128-135.
- Ruiz-Bailén M, Aguayo de, Serrano-Córcoles M, Diáz-Castellanos M, Ramos-Cuadra J, Reina-Toral A. Efficacy of thrombolysis in patients with acute myocardial infarction requiring cardiopulmonary resuscitation. Intensive Care Med. 2001;27(6): 1050-1057.
- Richling N, Herkner H, Holzer M, Riedmueller E, Sterz F, Schreiber W. Thrombolytic therapy vs primary percutaneous intervention after ventricular fibrillation cardiac arrest due to acute ST-segment elevation myocardial infarction and its effect on outcome. Am J Emerg Med. 2007 Jun;25(5):545-50. doi: 10.1016/j.ajem.2006.10.014. PMID: 17543659.
- Böttiger B, Bode C, Kern S, et al. Efficacy and safety of thrombolytic therapy after initially unsuccessful cardiopulmonary resuscitation: a prospective clinical trial. Lancet. 2001;357(9268):1583-1585.
Procainamide for Wide Complex Tachycardia
Digoxin Poisoning Management
Push Dose Vasopressors
Patient Case
- The team gets a call that there is a 75 year old male that triggered a sepsis alert in route with EMS and is currently desaturating on 15 L of oxygen with decision made to intubate this patient
- Prior to intubation, the patient hasn’t responded to a NS bolus infusion these are the patient’s vitals:
- Knowing that pre-intubation hypotension has been associated with peri-intubation cardiac arrest, which agent do you order? If it is not commercially available, how do you make it?
Pharmacology
| Phenylephrine (PE) | Epinephrine (EPI) | |
| Properties | A1 ++++ ↑ BP B1 ± ↔HR B2 ± | A1 +++ ↑ BP B1 +++++ ↑ HR B2 +++++ |
| Dose | 100-200 mcg PRN Q 1-5 minute | 10- 20 mcg PRN Q 1-5 minute |
| Formulation | Premixed Syringe- 1000 mcg/10 ml | Not commercially available |
| PK/PD | Onset: 1 minute Duration: ~10-20 minutes | Onset: 1 minute Duration: ~5-10 minutes |
| Adverse Effects | Reflex bradycardia Hypertension | Tachycardia Hypertension |
| Precautions | Bradycardia, heart block, heart failure, angina, acute MI | Tachycardia |
| Compatibility | Compatible with NS, LR, D5 | Compatible with NS, LR, D5 |
| Location in GHS | CPR, Trauma, Zone 2+3 Pyxis | 1 mg/ml: CPR, Trauma, Zone 2+3 Pyxis |
| Comments | Administer through a large bore peripheral IV; Low extravasation risk | Administer through a large bore peripheral IV; Low extravasation risk |
| Making Epinephrine and Phenylephrine the “EASY WAY” Supplies: 10 ml of NS, Insulin syringe, epinephrine or phenylephrine vial, tape, pen Instructions: |
| Making Epinephrine and Phenylephrine the Alternative Way Epinephrine Draw up 9 mL of normal saline into a 10 mL syringe (DO NOT use 10ml IV line “flush” syringes) Into this syringe, draw up 1 mL of EPINEPHphrine 0.1 mg/mL (1 mg/10ml) from a cardiac syringe |
Overview of Evidence
| Author, year | Design/ sample size | Intervention & Comparison | Outcome |
| Rotando, 2019 | Observational ED/ICU N=146 | PE 100 mcg/ mL or Ephedrine 50 mg/10 mL | Most common indication = peri-intubation hypotension Both agents associated with: ↑ SBP by 26 mmHg ↑ SBP by 26 mmHg ↓ HR by 6 beats per minute |
| Schwartz, 2016 | Observational ED N=76 | PE 100 mcg/ mL (pre-filled syringe) | 46.5% patients were initiated on vasopressor drip ≤ 30 minutes; mean MAP ↑ from 56.5 to 79.3 mmHg most common dose 100 mcg most common indication = peri-intubation hypotension |
| Panchal, 2015 | Observational ED N=119 | PE 100 mcg/1 mL | PE given during the peri-intubation period: ↑ SBP by 20 mmHg, ↑ DBP by 10 mmHg, HR unchanged |
| Doherty, 2012 | RCT OR N=60 | PE IV push 120 mcg (pre-filled syringe) Vs PE infusion @ 120 mcg/min | The infusion used more drug ( 1740 v 964 mcg) Push dose pressor had favorable impact of MAP compared to infusion |
References
- Micromedex [Electronic version].Greenwood Village, CO: Truven Health Analytics. Retrieved March 18, 2019, from http://www.micromedexsolutions.com/
- Scott Weingart. EMCrit Podcast 205 – Push-Dose Pressors Update. EMCrit Blog. Published on August 7, 2017. Accessed on March 19th 2019. Available at [https://emcrit.org/emcrit/push-dose-pressor-update/ ]
- Holden D. Ann Emerg Med. 2018 Jan;71(1):83-92.
- Panchal AR. J Emerg Med. 2015 Oct;49(4):488-94.
- Rotando A. Am J Emerg Med. 2019 Mar;37(3):494-498.
- Doherty A. Anesth Analg. 2012 Dec;115(6):1343-50.
- Schwartz MB. Am J Emerg Med. 2016 Dec;34(12):2419-2422
Sodium Bicarbonate in Cardiac Arrest
Introduction
- Out-of-hospital cardiac arrest (OHCA) remains a leading cause of mortality and a substantial issue of public health concern worldwide.
- Sodium bicarbonate (SB) administration has been considered an important part of treatment for severe metabolic acidosis in cardiac arrest, because based on pathophysiologic considerations, normalization of extracellular and intracellular pH was considered a meaningful endpoint of resuscitation.
- Correction of metabolic acidosis with SB was recommended by early advanced cardiac life support (ACLS) guidelines published in 1973, and SB was the medication most frequently used during cardiac arrest until mid-1980s
- The 2010 ACLS Guidelines for adults published by the American Heart Association (AHA) state that “Routine use of sodium bicarbonate is not recommended for patients in cardiac arrest” (class lll recommendation, based on level of evidence (LOE) B)
Pharmacology
| Dose | 0.5-1 meq/kg/dose • Repeat doses should be guided by arterial blood gases | ||
| Administration | IV injection during cardiac arrest | ||
| PK/PD | Onset Iv: Rapid Duration IV: 8-10mins Excretion: Urine (<1%) | ||
| Adverse Effects | Hypocalcemia Intracellular acidosis (without adequate ventilation) HYPERNATREMIA Hyperosmosis Shift O2 release by hemoglobin | ||
| Compatibility | Sodium bicarbonate solution may inactivate catecholamines such as epinephrine | ||
- May decrease of the biological effect of epinephrine to 77- 82 % of nonalkaline solution
- not powered
Overview of Evidence
| Author, Year | Design/ sample size | NaHCO3 regimen | Outcome |
| Chen YC, 2018 | Observational/ n=5589 | Not reported | Sodium bicarbonate during ED resuscitation was significantly associated with an increased rate of survival to hospital admission. |
| Kawano T, 2017 | Prospective observational/ n=13,865 | Not reported | In OHCA patients, prehospital SB administration was associated with worse survival rate and neurological outcomes to hospital discharge. |
| Ahn S, 2017 | RCT/ n=50 | 50 mEq/L vs Placebo | No difference in sustained ROSC (4% vs 16%) or good neurological outcome (0% vs 4% , p=.1) SB had significant effect on pH (6.99 vs. 6.90, P=0.038) and bicarbonate levels (21.0 vs. 8.0 mEq/L) |
| Wang CH, 2016 | Retrospective observational study/ n=109 | Not Reported | SB was positively associated with sustained ROSC when serum potassium level was <7.9 mEq in IHCA Calcium and SB was positively associated with sustained ROSC when serum potassium level <9.4 mEq/L IHCA |
| Vukmir RB, 2005 | RCT/ n=792 | 1 mEq/kg NaHCO3 | Overall survival rate was 13.9% No difference in survival in those who received bicarbonate 2-fold increase in survival in arrest >15 min (32.8 vs 15.4)* |
| Bishop RL, 1976 | Animal+human case studies/ n=6 | 1 mEq/kg of 7.5% sodium bicarbonate in dogs 0.5-0.9 mEg/kg in humans | Animal 1 mEq/Kg SB resulted in increases in the Pco2 (27→49), pH (7.38 →7.56) and the serum osmolality (309→349) Man 0.5-0.9 mEq/Kg SB resulted in increases in the Pco2 (24.5→38.8), pH (7.23 →7.48) and the serum osmolality (308→343) |
References
- Sodium bicarbonate. Micromedex [Electronic version].Greenwood Village, CO: Truven Health Analytics. Retrieved October 11, 2018, from http://www.micromedexsolutions.com/
- Bishop RL, et al. Sodium bicarbonate administration during cardiac arrest. Effect on arterial pH PCO2, and osmolality. JAMA. 1976 Feb 2;235(5):506-9.
- Vukmir RB, et al. Sodium bicarbonate in cardiac arrest: a reappraisal. Am J Emerg Med. 1996 Mar;14(2):192206.
- Vukmir RB, et al. Sodium bicarbonate improves outcome in prolonged prehospital cardiac arrest. Am J Emerg Med. 2006 Mar;24(2):156-61.
- Wang CH,et al. The effects of calcium and sodium bicarbonate on severe hyperkalaemia during cardiopulmonary resuscitation: A retrospective cohort study of adult in-hospital cardiac arrest. Resuscitation. 2016 Jan;98:105-11.
- Ahn S, et al. Sodium bicarbonate on severe metabolic acidosis during prolonged cardiopulmonary resuscitation: a double-blind, randomized, placebo-controlled pilot study. J Thorac Dis. 2018 Apr;10(4):22952302
- Kawano T, et al. Prehospital sodium bicarbonate use could worsen long term survival with favorable neurological recovery among patients with out-of-hospital cardiac arrest. Resuscitation. 2017 Oct;119:63-69.
- Chen YC, et al. The association of emergency department administration of sodium bicarbonate after out of hospital cardiac arrest with outcomes. Am J Emerg Med. 2018 Mar 5. pii: S0735-6757(18)30187-6.
How Space Learning helps you pass board certification exams
Unleash the Power of Spaced Repetition for Pharmacist Board Certification Exams
Outline
Introduction
A. What is Spaced Repetition?
B. Benefits of Spaced Repetition for Pharmacist Board Certification Exams
II. How to Implement Spaced Repetition Strategies
A. Create a Study Plan and Set Regular Review Points
B. Tailor the Study Plan to Your Learning Style
C. Focus on Strengthening Weak Areas
III. Conclusion
A. Maximizing Exam Scores with Spaced Repetition Strategies
B. Final Thoughts on Using Spaced Repetition for Board Certification Exams
Introduction
Are you preparing for your Pharmacist Board Certification Exam? If so, you need to study effectively so you can make the most of your time and maximize your exam score. One way to do this is by using spaced repetition – an evidence-based learning technique proven to increase the rate of learning. In this blog post, we will discuss the benefits of spaced repetition for Pharmacist Board Certification Exams, how to implement it, and some tips on maximizing your exam score with space repetition strategies. So let’s dive in!
What is Spaced Repetition?
Spaced repetition is an evidence-based learning technique that is usually performed with flashcards or questions. It involves deliberately spacing out the time spent studying a specific topic or material in order to better retain the knowledge. Newly introduced and more difficult questions are shown more frequently, while older and less difficult flashcards are shown less frequently in order to exploit the psychological spacing effect. The use of space repetition has been proven to increase the rate of learning by helping students to better retain information over time. It can be used effectively in many contexts, including for pharmacist board certification exams. By using space repetition, pharmacists can ensure that they are consistently revisiting the material they need to know and strengthening their understanding of the topics. This can ultimately lead to improved exam performance and a successful board certification.
Benefits of Spaced Repetition for Pharmacist Board Certification Exams
Spaced repetition is an excellent tool for pharmacist board certification exams, as it can help to increase the rate of learning and improve performance on the exam. It can also be used to reinforce knowledge and strengthen understanding of concepts. By utilizing space repetition strategies, pharmacists can ensure that they are reviewing material in a way that is tailored to their individual needs and learning styles. By scheduling regular review sessions, pharmacists can ensure that all of the material has been thoroughly understood. This will ultimately lead to improved exam scores and better overall performance in the board certification process. Additionally, space repetition is a great way to focus on weaker areas of knowledge, allowing pharmacists to spend their studying time on topics that need more work. In this way, space repetition can be used to maximize the effectiveness of studying for board certification exams.
How to Implement Spaced Repetition Strategies
In order to effectively use space repetition strategies for pharmacist board certification exams, it is important to create a comprehensive study plan that incorporates space repetition. First, pharmacists should break down the material into smaller, more manageable chunks and create a timeline for studying each section. This timeline should be tailored to the individual’s learning style and include regular review points for space repetition. It is important to space out those reviews in order to maximize their effectiveness, as this will allow pharmacists to fully understand and retain the material. Additionally, space repetition should be used to focus on weaker areas of knowledge and ensure that those topics are being thoroughly reviewed. By creating a comprehensive space repetition strategy and sticking to it, pharmacists can ensure that they are fully prepared for their board certification exam.
Conclusion
Spaced repetition is an evidence-based learning technique that can be used effectively to maximize exam scores for pharmacist board certification exams. By utilizing space repetition strategies, pharmacists can ensure that they are consistently revisiting material and reinforcing their understanding of the topic. This will ultimately lead to improved performance on the exam and better overall outcome in the board certification process. Additionally, space repetition is a great way to focus on weaker areas of knowledge and ensure that those topics are being thoroughly reviewed. In this way, space repetition can be used to maximize the effectiveness of studying for board certification exams.
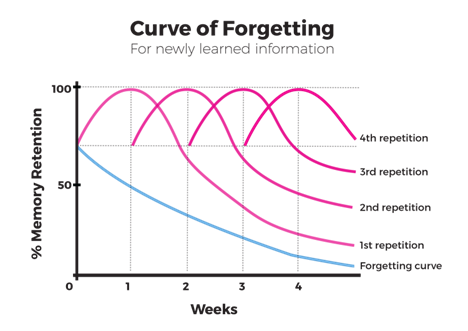

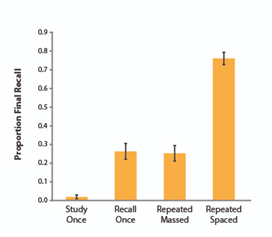
Repeated retrieval with long intervals between each test produced a 200% improvement in long-term retention relative to repeated retrieval with no spacing between tests
Reference: How To Remember What You Learn For Longer With Spaced Repetition. https://blog.alexanderfyoung.com/how-to-remember-what-you-learn-for-longer-with-spaced-repetition/
How the BCEMP Test is Administered and What Is On It?
Preparing for the BCEMP Exam: What You Need to Know about the Exam
1. Introduction
2. Overview of the BCEMP Exam
3. Over of Domains of BCEMP EXAM
4. Conclusion
Introduction
The Board Certified Emergency Medicine Pharmacist (BCEMP) exam is a rigorous assessment of emergency medicine knowledge and understanding. As an essential component for those seeking professional success within the field, this 4-hour and 23 minutes, computer-based test covers topics such as pharmacology, patient assessment, disease state management, and emergency department protocols. Knowing what to expect on the exam and how to properly prepare for it is key to passing with flying colors. This article provides an overview of the BCEMP exam and offers strategies for success. From understanding the domains covered, to reviewing relevant material, this guide will equip you with the knowledge necessary for approaching the BCEMP exam with confidence. Read on to learn more about this essential test and take the first step towards professional advancement.
BCEMP Exam Overview
The BCEMP exam is divided into three domains. Domain 1: Patient Care and Management covers topics such as patient assessment, diseases state management, pharmacology, medications, and other related issues. Domain 2: Practice Management focuses on the delivery of emergency care services including review adverse drug events and medication errors, quality assurance activities, drug shortages, drug shortages, emergency/disaster preparedness planning, and practice advancement and growth. Domain 3: Education and Research looks into the delivery of patient education and research skills in emergency medicine. A successful completion of the BCEMP exam can be used to demonstrate mastery in emergency medicine topics and may lead to increased professional opportunities. It is important to properly prepare for the BCEMP exam by studying resources provided by the Board of Specialty Pharmacy. The exam is 175 questions , multiple-choice and is based on the content outline released by the Board. The length of the exam is 4 hours and 23 minutes. Taking the time to study for this exam adequately can ensure candidates are positioned for success on their certification journey.
Domains of BCEMP EXAM
Domain 1: Patient Care and Management covers patient assessment, disease state management, pharmacology, medications, and other related issues. This is 75% of the exam or 131 questions on the certification exam and is mostly pharmacotherapy. This included your disease state management, drug information, and preparation and procurement activities. The subdomain items are listed below
- Participate in the bedside management of medical emergencies (e.g., trauma, stroke, psychiatric, toxicological) and resuscitations to optimize the medication use process.
- Identify and prioritize (triage) Emergency Department patients by analyzing the relevant acuity indices and opportunities for optimization of pharmacotherapy.
- Collect essential patient information (including patient history, medication use) by utilizing available resources (e.g., pre-hospital providers).
- Identify and evaluate medication-related problems based on clinical presentation, available history, or laboratory data.
- Contribute to the formulation of a differential diagnosis in the setting of limited information. 1.06 Design pharmaceutical care plan utilizing available patient-specific information and best available evidence to provide patient and family-centered care.
- Recommend and support implementation of the pharmaceutical care plan in the Emergency Department.
- Expedite the preparation/procurement and administration of time-sensitive therapeutic regimens.
- Make evidence-based recommendations for alternative routes of administration.
- Monitor and evaluate patient response to initial therapy and re-design treatment plan as necessary.
- Serve as the primary source of drug information for all practitioners and patients within the Emergency Department.
- Ensure continuity of care during healthcare transition and across levels of care.
- Identify and seek appropriate outside resources available to assist in the management of the Emergency Department patient.
Domain 2: Practice Management focuses on the delivery of emergency care services including review adverse drug events and medication errors, quality assurance activities, drug shortages, drug shortages, emergency/disaster preparedness planning, and practice advancement and growth. we can think of this as part of your day when you’re replying to emails, making protocols, reviewing medication safety events, and dealing with stocking your automatic dispense cabinets with medications that may or may not be on shortage. Domain 2 represents 15% of the exam or 26 questions on the certification exam. The subdomain items for domain 2 is below.
- 2.01 Anticipate, monitor, detect, report, and review adverse drug events and medication errors. 2.02 Recognize trends, system failures, and gaps in the medication use process, and perform quality assurance activities (e.g., MUE) that promote safe and effective medication use.
- 2.03 Ensure a process to maintain and optimize inventory and availability of medications essential to provide timely care in the Emergency Department.
- 2.04 Ensure an appropriate process exists for medication order review in the Emergency Department.
- 2.05 Assist the organization in achieving compliance with accreditation, legal, regulatory, and safety requirements related to the medication use process.
- 2.06 Contribute to contingency planning that addresses limited availability of critical drugs that affect patients in the Emergency Department (e.g., drug shortages, emergency preparedness). 2.07 Participate in emergency/disaster preparedness planning or response activities.
- 2.08 Develop, maintain, monitor, and support evidence-based medication use guidelines and pathways to assure safe and cost-effective medication use.
- 2.09 Identify and implement opportunities for practice advancement and growth within the Emergency Department (e.g., collaborative practice agreements, public health initiatives, expanded coverage).
- 2.10 Advocate for and justify emergency medicine pharmacy services.
Domain 3: Education and Research look into the delivery of patient education and research skills in emergency medicine. This is probably the code name for some biostatistics and research designs here. Most of this will need a little touching on if you’re not actively involved in research. Domain 3 represents 10% of the exam or 18 questions on the certification exam. The subdomain items are listed below
- 3.01 Provide emergency medicine professionals and trainees. — focused education, training, or mentoring for healthcare
- 3.02 Educate patients and caregivers using appropriate techniques tailored to the audience, with a focus on high risk medications or where the visit resulted from an adverse drug event.
- 3.03 Participate in continuous professional development related to emergency pharmacy practice (e.g., professional organizations, continuing education, clinical pharmacy networks).
- 3.04 Retrieve and critically evaluate biomedical literature and other sources regarding study design methodology, statistical analysis, and applicability of study results to emergency medicine. 3.05 Contribute to the body of knowledge in the field of emergency medicine
Conclusion
In conclusion, the BCEMP exam is a comprehensive test that covers all aspects of emergency medicine, from patient care to practice management and education and research. Preparing for the test requires an understanding of the content domains and subdomains, as well as a thorough review of related materials. With proper preparation and dedication, individuals can successfully pass the BCEMP exam and become certified in emergency medicine. Good luck!
The BCEMP exam is a challenging test, but with the right preparation, anyone can become certified in emergency medicine.
Good luck!
Jimmy L. Pruitt III, PharmD, BCPS, BCCP
Emergency Medicine Clinical Pharmacy SPeacialist
The Best Practices for Passing the Pharmacy Board Certification Exam
I. Introduction
II. Review the Topics Covered by the Exam
III. Decide Which Study Materials to Use
IV. Create a Study Plan or Schedule
V. Stay Motivated and Track Your Progress
VI.Conclusion
Introduction
Are you looking to take the pharmacy board exam? Becoming certified is an important step towards a successful career as a pharmacist and requires proper preparation. This guide will provide you with all the information you need to know about studying for the pharmacy board certification exam, from which materials to use to creating an effective study plan. With these tips and strategies, you can be well on your way to passing the pharmacy board exam!
Review the topics covered by your chosen board examination
When studying for the pharmacy board certification exam, it is important to review the topics covered by your chosen board examination. This will help you determine what material will be tested on the exam so you can focus your study efforts and make sure that you are adequately prepared. Generally, these exams cover a variety of topics such as pharmacology, drug therapy, pharmacy law and ethics, compounding, and pharmacokinetics. It is also important to be aware of any prerequisites or continuing education credits that may need to be completed before taking the exam.
Additionally, you should make sure to access relevant study materials that are specific for your board certification examination. Doing so will help ensure that you have all the information you need to successfully pass the exam.
Decide which study materials are best for you
When deciding which study materials are best for you, it is important to choose materials that are approved by your chosen board examination. This will help ensure that the material you are studying is accurate and up to date with the latest information. You can find these materials on websites such as the ASHP, ACCP, Pharmacy & Acute Care University or through continuing education classes.
Additionally, consider utilizing study guides, practice tests, and other resources such as online discussion forums to help you stay on track. The material you choose should be tailored to your specific board exam so that you can focus your studying for optimal results.
Create a study plan or schedule
Creating a study plan or schedule is an essential part of preparing for the pharmacy board certification exam. Start by selecting a realistic completion date and setting smaller goals along the way. Breaking up your studying into manageable chunks can help make it easier to stay on track and motivated.
Additionally, consider utilizing online tools such as a calendar or task list to keep you organized and accountable. Make sure to set aside plenty of time for practice questions and review material. This will help you become familiar with what to expect on the exam and ensure that you have mastered all the material before taking it.
Stick with your plan and stay motivated
Once you have created your study plan, it is important to stick with it and stay motivated. This can be challenging, especially if you have a busy schedule or other commitments. However, consistency is key when it comes to studying for the pharmacy board certification exam. Make sure to set aside ample time each day to focus on your studies and give yourself breaks when needed. Additionally, consider finding a study partner or forming a study group to help keep you accountable and motivated. Finally, don’t forget to reward yourself when you reach your goal so that you have something to look forward to while studying.
Conclusion
Passing the pharmacy board certification exam can be a challenging but rewarding experience. Seeking advice and support from other pharmacists can help make the process easier. Connecting with other pharmacists, whether it’s through online discussion forums or in person, can provide valuable insight and guidance that can help you succeed. Don’t be afraid to ask questions and take advantage of the wisdom of other pharmacists who have been through the process before you. With their help and support, you can feel confident as you prepare for your pharmacy board certification exam.
Good luck!
What are the Pass rates for BPS Exams?
Uncovering the Success Rates of Board Certification Exams for Specialty Pharmacists
Are you considering a career in specialty pharmacy? If so, it is important to understand the pass rates of board certification exams for this field. Board-certified specialty pharmacy certifications offer pharmacists additional training and expertise in specific areas of practice. In this article, we will explore the overall and first time pass rates for Board-Certified Critical Care Pharmacist (BCCCP) and Board-Certified Pharmacotherapy Specialist (BCPS). We will also provide useful information to help you understand the importance of obtaining specialty pharmacy certification.
Pass Rates
In this administration window, a total of 2,757 out of 4,272 examinees were successful in one of thirteen certification examinations or nine recertification examinations.
- Board-Certified Critical Care Pharmacist (BCCCP) has a pass rate of 73% and a first-time pass rate of 82% in the most recent examination period.
- Board-Certified Pharmacotherapy Specialist (BCPS) has a pass rate of 63% and a first-time pass rate of 72% in the most recent examination period.
These results demonstrate that pharmacists who take the relevant exams are generally successful, though they may require additional preparation depending on their field.
The statistics indicate that the exams are not easy and require a significant amount of preparation. Pharmacists should consider taking additional courses or engaging in self-study to ensure they pass the certification examinations with flying colors. Additionally, pharmacists should have experience working in their respective field before taking any board certification exam in order to better prepare themselves for the exams. It is recommended that pharmacists research the requirements for their respective certifications and begin preparing at least 3-6 months before the examination date.
The Benefits of Obtaining Board-Certified Specialty Pharmacy Certification
Becoming board-certified in a specialty field of pharmacy has many advantages. For example, pharmacists who are certified may receive higher salaries and better job opportunities. They can also help patients manage their medications more effectively and provide improved care. Furthermore, being certified is an important step to advancing one’s career and becoming a leader in the field.
Other Pass Rates
Board-Certified Critical Care Pharmacist (BCCCP) 73%
Board-Certified Cardiology Pharmacist (BCCP) 54%
Board-Certified Infectious Diseases Pharmacist (BCIDP) 73%
Board-Certified Nutrition Support Pharmacist (BCNSP) 93%
Board-Certified Oncology Pharmacist (BCOP) 57%
Board-Certified Pediatric Pharmacy Specialist (BCPPS) 66%
Board-Certified Pharmacotherapy Specialist (BCPS) 63%
Board-Certified Psychiatric Pharmacist (BCPP) 52%
Board-Certified Transplant Pharmacist (BCTXP) 43%
In conclusion, specialty pharmacy certifications open up new opportunities to those who have the dedication and commitment to pursue them. With a pass rate of 73% for Board-Certified Critical Care Pharmacists (BCCCP) and 63% for Board-Certified Pharmacotherapy Specialists (BCPS), pharmacists who take the relevant exams are generally successful. Becoming certified provides numerous benefits such as higher salaries, better job opportunities, and improved patient care. Pharmacists should take the time to research the requirements for their respective certifications and begin preparing at least 3-6 months before the examination date in order to maximize their chances of success. With dedication, any pharmacists can achieve board certification status in a specialty field of pharmacy.
References:
Big Changes in Blood Pressure: A Simple Guide to the 2025 Hypertension Guidelines
The way doctors and pharmacists manage high blood pressure is about to change. The new 2025 AHA/ACC Hypertension Guidelines have been released, introducing significant, evidence-based updates designed to improve patient safety and provide more effective care.
Whether you are a patient or a healthcare provider, it’s important to understand these key shifts. Here’s a simple breakdown of what you need to know.
1. “Hypertensive Urgency” Gets a New Name and a Safer Approach
One of the biggest changes is the terminology. The term “hypertensive urgency” is now being replaced with
“severe hypertension”. This refers to a blood pressure reading higher than 180/120 mm Hg in a patient
without symptoms of acute target organ damage.
Why the change? The old term often led to unnecessary emergency department visits and the use of potent IV medications that could lower blood pressure too quickly, causing harm. The new approach for patients with asymptomatic severe hypertension is to:
- Avoid IV medications in the hospital or ED.
- Start well-tolerated oral medications.
- Arrange for a follow-up appointment with a primary care provider or cardiologist within a few days.
2. A Smarter Way to Decide Who Needs Medication: The PREVENT Calculator
The new guidelines integrate the
PREVENT risk calculator, a more accurate and inclusive tool for predicting a person’s 10-year risk of heart attack or stroke. This calculator includes factors like kidney disease and social determinants of health to better guide treatment decisions.
The new rules are:
- High-Risk Patients: If you have established cardiovascular disease, diabetes, chronic kidney disease, or a PREVENT risk score of 7.5% or higher, medication is now recommended if your blood pressure is 130/80 mm Hg or higher.
- Lower-Risk Patients: If your blood pressure is between 130-139/80-89 mm Hg and your risk score is less than 7.5%, the first step is a 3-6 month trial of lifestyle changes. Medication is only recommended if blood pressure remains high after that period.
3. New Rules for Stroke and Brain Bleeds
The guidelines provide critical updates for managing blood pressure during neurological emergencies:
- After an Ischemic Stroke (Post-Reperfusion): The guidelines now state that lowering systolic blood pressure below 140 mm Hg in the first 24-72 hours can be harmful and should be avoided. The goal is to maintain pressure between 140-180 mm Hg to ensure the brain gets enough blood flow to recover.
- For a Brain Bleed (ICH): If the systolic pressure is between 150-220 mm Hg, the new target is to lower it to 130-140 mm Hg within the first 7 days. For extremely high pressures (>220 mm Hg), a continuous IV infusion is recommended over single “bolus” injections to prevent dangerous blood pressure swings.
4. Critical Updates for Managing Hypertension in Pregnancy
The 2025 guidelines emphasize safer and more proactive care for pregnant patients:
- Treat Urgently: Severe hypertension (BP ≥160/110 mm Hg) during pregnancy is a medical emergency. Treatment must be started within 30-60 minutes to prevent a maternal stroke.
- Treat Earlier: For chronic hypertension in pregnancy, treatment should now begin when blood pressure is 140-159/90-109 mm Hg to a target of <140/90 mm Hg.
- Preeclampsia Prevention: Low-dose aspirin (81 mg daily) is strongly recommended for pregnant patients with chronic hypertension, starting at 12 weeks of gestation, to reduce the risk of preeclampsia.
- Medication Safety: The list of contraindicated medications has been expanded. Common drugs like ACE inhibitors (e.g., lisinopril), ARBs (e.g., losartan), and the beta-blocker atenolol should be avoided during pregnancy due to risks to the fetus.
Guideline Resources
These updates represent a major step forward in hypertension management. For healthcare professionals seeking more information, the following resources are available:
- Download the Pharmacist’s Guide: Comprehensive Clinical Reference: 2025 AHA/ACC Hypertension Guidelines for Pharmacists
- Read the Full Guideline: 2025 Guideline for the Management of High Blood Pressure in Adults (AHA/ACC)
PubMed Search Guide for Pharmacists
🔬 PubMed Search Guide for Pharmacists
Master evidence-based drug therapy research with advanced search strategies
🎯 Core Concepts You’ll Use Every Time
A. MeSH (Medical Subject Headings)
What: PubMed’s controlled vocabulary for indexing citations (e.g., Septic Shock[MeSH], Drug Interactions[MeSH]). Searching with MeSH enhances precision and recall by unifying synonyms under a single concept.
Pharmaceutical Preparations [MeSH]
├── Dosage Forms [MeSH]
├── Drug Combinations [MeSH]
└── Pharmaceutical Solutions [MeSH]
B. Essential Field Tags for Pharmacists
Title only
High precision
Title OR Abstract
Balanced approach
MeSH heading
Controlled vocabulary
Author
Find specific researchers
C. Boolean Logic & Critical Behavior
✅ Good Practice
Uses OR to combine synonyms within a concept
❌ Poor Practice
Missing Boolean operator – unpredictable results
💊 Essential Pharmacy MeSH Terms
Core Pharmaceutical Concepts
Main term for DDIs
ADME processes
Drug effects
Metabolism enzymes
Clinical pharmacy practice
Patient safety
Therapeutic monitoring
Multiple medications
Clinical Conditions Pharmacists Encounter
ICU pharmacy
Ambulatory care
Community pharmacy
Cardiology pharmacy
Dose adjustments
Hepatic impairment
🔍 Advanced Search Strategies
Study Design Filters
This is the gold standard for finding RCTs in PubMed, validated by Cochrane.
Use for real-world evidence and outcomes research.
Perfect for evidence-based guidelines and protocols.
Date Limiting Strategies
Two Approaches to Date Limiting:
1UI Method: Use sidebar → Publication Dates → Custom range (e.g., 2019-2025)
2Query Method: Include in your search string:
📝 Comprehensive Worked Examples
Example 1: Vasopressin in Septic Shock
Clinical Context:
Norepinephrine is first-line; vasopressin is second-line. The 2025 OVISS study suggests earlier vasopressin initiation.
1Broad Seed Search (MeSH + tiab):
2RCT-Focused Version:
Example 2: Drug-Drug Interactions with Warfarin
Clinical Scenario:
Community pharmacist needs evidence on clinically significant warfarin interactions.
Example 3: Medication Adherence in Diabetes
Clinical Question:
What interventions improve medication adherence in diabetic patients?
⚠️ Drug Interaction Research Strategies
Key MeSH Terms for Drug Interactions
Primary term
Additive effects
Opposing effects
Metabolism interactions
Transport interactions
Nutrition interactions
Common CYP450 Interaction Searches
Specific Interaction Examples
Grapefruit-Drug Interactions:
📋 Copy-Paste Templates
A. Therapy/RCT Template
B. Observational Template
C. Drug Interaction Template
D. Pharmacokinetics Template
🔧 Troubleshooting & Pro Tips
Common Issues & Solutions
• Add field tags ([ti] for key terms)
• Include MeSH subheadings
• Apply Article Type, Humans, and Date filters
• Use Narrow option in Clinical Queries
• Remove quotes to re-enable ATM
• Use OR to include more synonyms
• Combine MeSH with [tiab]
• Check spelling and try broader terms
• Try proximity: “term A term B”[tiab:~0]
• Drop quotes and use field tags
• Check Search Details for interpretation
• Use Advanced → History to combine sets
• Save final strategy for future use
• Document your search approach
• Share search strings with colleagues