Clinical Content
6 min read
October 6, 2023
6 min read
October 6, 2023
Penicillin Allergy Cross Reactivity
J
Jimmy
PharmD
Introduction
- Only 0.5% to 2% of patients with a documented penicillin allergy that are administered a penicillin will exhibit a hypersensitivity reaction, usually presenting as a rash or hives.
- True IgE-mediated penicillin allergies that cause anaphylaxis are rare.
- An IgE-mediated penicillin allergy can diminish over time, as 80% of patients become tolerant after a decade.
- Patients with a documented penicillin allergy may be inappropriately exposed to alternative antibiotics, resulting in increased treatment failures, adverse effects, and antimicrobial resistance.
- Penicillins, cephalosporins, and carbapenems all share a beta-lactam core structure, thus raising the potential for cross-reactivity among these agents.
Pharmacology
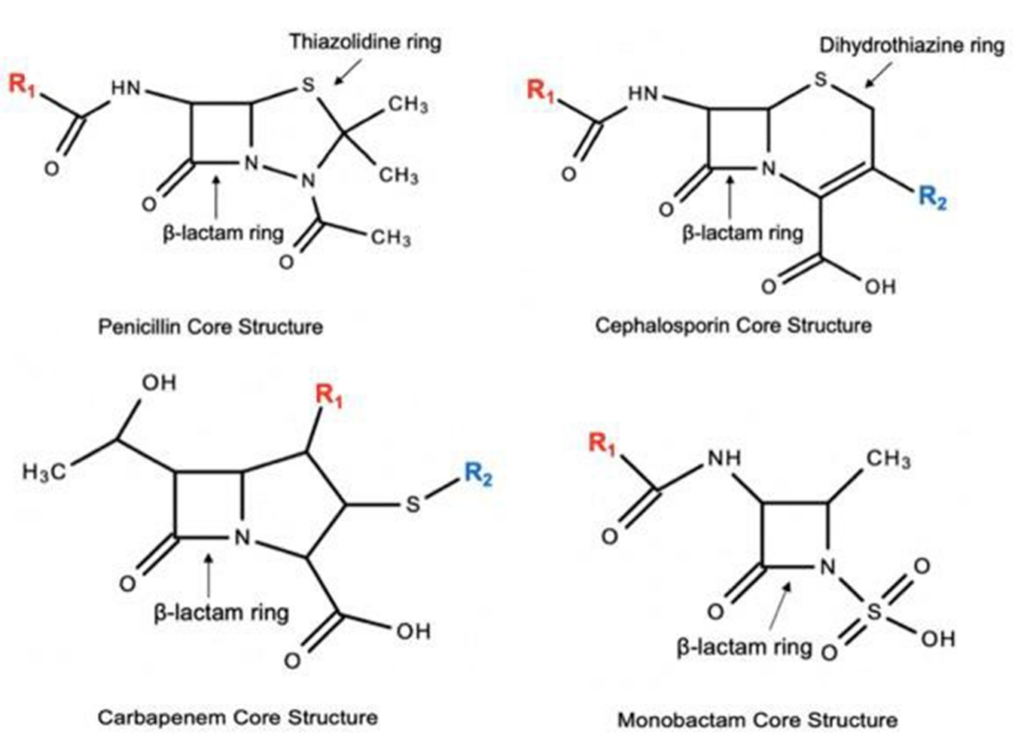
- The following drugs in each group may have cross-reactivity to each other due to similar side chains
- Cross-reactivity between penicillins and cephalosporins is about 2%
- Cefazolin is NOT likely to cross react with penicillin (side chains NOT similar)
- Cross-reactivity with monobactams (i.e. aztreonam) is negligible
- Cross-reactivity between penicillins and carbapenems is <1%
| Group 1 | Group 2 | Group 3 | Group 4 |
| Penicillin Cefoxitin Cefuroxime |
Amoxicillin Ampicillin Cefaclor Cephalexin Cefadroxil |
Ceftriaxone Cefotaxime Cefuroxime Cefepime Cefpodoxime Ceftaroline |
Aztreonam Ceftolazane Ceftazidime |
Overview of Evidence
| Author | Design | Intervention & Comparison | Outcome | |
| Why Cross-Reactivity? | ||||
| Nagakura, 1990 Mayorga, 1995 | Animal study | -Studied antibodies formed when animals were immunized with protein-beta-lactam conjugates | -92% of the antibodies recognized an epitope in which the side chain was the main constituent -The side chain is the most important determinant in penicillin immunogenicity | |
| Cephalosporins | ||||
| Goodman, 2001 | Retrospective review (n=2933) | -Orthopedic patients with penicillin allergy receiving cefazolin prior to a procedure | Only 1 patient may have had an allergic reaction to cefazolinCross-reactivity rate with cefazolin was 0.33% | |
| Daulat, 2004 | Retrospective review (n=606) | -Patients with penicillin allergy receiving cephalosporins -42% 1st gen., 21% 2nd gen., and 37% 3rd or 4th gen. cephalosporins | Only 1 patient had an allergic reaction that was documented as worsening of underlying eczema after being placed on cefazolinCross-reactivity was 0.17% | |
| Apter, 2006 | Retrospective review (n=3920) | -Patients with a prescription for penicillin followed by a prescription for a cephalosporin -Identified allergic-like events within 30 days after each prescription | Only 43 patients who experienced an allergic- like reaction after both penicillin and cephalosporinCross-reactivity rate was 1.1%70% of these patients just had urticariaThe risk of anaphylaxis to cephalosporins was only 0.001% | |
| Romano, 2018 | Prospective review (n=252) | Prospective study of 252 subjects with IgE-mediated hypersensitivity to penicillins – Serum specific IgE assays for cefaclor and skin tests for 10 cephalosporins -Oral challenges with cefuroxime axetil, ceftriaxone, cefaclor, and cefadroxil for subjects with negative skin tests | 99 subjects (39.3%) had positive allergy tests for cephalosporins 95 subjects (37.7%) were positive to aminocephalosporins and/or cefamandole, which share side chains with penicillins All 244 subjects who underwent challenges with cefuroxime axetil and ceftriaxone tolerated them 7 subjects reacted to cefaclor or cefadroxil | |
| Carbapenems | ||||
| Romano, 2006 | Prospective study (n=112) | -Skin tested to penicillins and then skin tested to imipenem -If skin test to imipenem was negative, then challenged with IM dose | Only 1 patient of the penicillin skin-test positive patients had a positive skin test to imipenemCross-reactivity rate was 0.9%None of the 110 patients with a negative imipenem skin test that underwent IM challenge had a reaction | |
| Romano, 2007 | Prospective study (n=104) | -Skin tested to penicillins and then skin tested to meropenem -If skin test to imipenem was negative, then challenged with IV dose | Only 1 patient of the penicillin skin-test positive patients had a positive skin test to meropenemCross-reactivity rate was 1%All 103 patients with a negative meropenem skin test tolerated the IV challenge | |
| Atanaskovic- Markovic, 2008 | Prospective study (n=108) | -Children with penicillin allergy were skin tested to penicillin and meropenem -If skin test to meropenem was negative, then challenged with IV dose | Only 1 patient with a positive penicillin test reacted to the meropenem skin testCross-reactivity rate was 0.9%All 107 patients with a negative meropenem skin test tolerated the IV challenge | |
| Sánchez de Vicente, 2020 | Prospective study (n=137) | Tolerance testing for cephalosporins and carbapenems in patients with confirmed penicillin allergy | 0/46 patients showed positive skin tests for imipenem. 0.79% (1/137) patients showed a positive skin test for cefuroxime.0.79% (1/137) patients showed a positive skin test for ceftriaxone. | |
Conclusions
- True penicillin allergies are less common than reported, and anaphylaxis is uncommon.
- Cross-reactivity among penicillins and cephalosporins is attributed to similarity in side chains.
- Cephalosporin cross-reactivity with penicillins is much lower than reported in early studies partly due to contamination of study drugs with penicillin.
- Cross-reactivity between cephalosporins is about 2% and with carbapenems is <1%
References
- Apter AJ, Kinman JL, Bilker WB, et al. Is There Cross-Reactivity Between Penicillins and Cephalosporins? Am J Med. 2006;119(4):354e11-19.
- Atanaskovic-Markovic M, Gaeta F, Medjo B, Viola M, Nestorovic B, Romano A. Tolerability of Meropenem in Children with IgE-Mediated Hypersensitivity to Penicillins. Allergy. 2008;63:237-240.
- Blumenthal KG, Shenoy ES, Wolfson AR, et al. Addressing Inpatient Beta-Lactam Allergies: A Multihospital Implementation. J Allergy Clin Immunol Pract. 2017;5(3):616-625.
- Blumenthal KG, Huebner EM, Fu X, et al. Risk-Based Pathway for Outpatient Penicillin Allergy Evaluations. J Allergy Clin Immunol Pract. 2019;7(7):2411-2414.
- Campagna JD, Bond MC, Schabelman E, Hayes BD. The Use of Cephalosporins in Penicillin-Allergic Patients: A Literature Review. J Emerg Med. 2012;42(5):612-620.
- Chaudry SB, Veve MP, Wagner JL. Cephalosporins: A Focus on Side Chains and Beta-Lactam Cross-Reactivity. Pharmacy. 2019;7:1-16.
- Daulat S, Solensky R, Earl HS, Casey W, Gruchalla RS. Safety of Cephalosporin Administration to Patients with Hstories of Penicillin Allergy. J Allergy Clin Immunol Pract. 2004;113(6):1220-1222.
- DePestel DD, Benninger MS, Danziger L, et al. Cephalosporin Use in Treatment of Patients with Penicillin Allergies. J Am Pharm Assoc. 2008;48:530-540.
- Goodman EJ, Morgan MJ, Johnson PA, Nichols BA, Denk N, Gold BB. Cephalosporins can be Given to Penicillin-Allergic Patients Who Do Not Exhibit an Anaphylactic Response. J Clin Anesth. 2001;13(8):561-564.
- Mayorga C, Obispo T, Jimeno L, et al. Epitope Mapping of Beta-Lactam Antibiotics with the Use of Monoclonal Antibodies. Toxicology. 1995;97:225-234.
- Nagakura N, Souma S, Shimizu T, Yanagihara Y. Anti-Ampicillin Monoclonal Antibodies and their Cross- Reactivities to Various Beta-Lactams. Br J Hosp Med. 1990;44:252-258.
- Romano A, Viola M, Gueant-Rodriguez RM, Gaeta F, Pettinato R, Gueant JL. Imipenem in Patients with Immediate Hypersensitivity to Penicillins. N Engl J Med. 2006;354:2835-2837.
- Romano A, Viola M, Gueant-Rodriguez RM, Gaeta F, Valluzzi R, Gueant JL. Brief Communication: Tolerability of Meropenem in Patients with IgE-Mediated Hypersensitivity to Penicillins. Ann Intern Med. 2007;146:266-269.
- Shenoy ES, Macy E, Rowe T, Blumenthal KG. Evaluation and Management of Penicillin Allergy: A Review. JAMA. 2019;321(2):188-199.
- Sánchez de Vicente J, Gamboa P, García-Lirio E, Irazabal B, Jáuregui I, Martínez MD, Segurola A, Seras Y, Galán C. Tolerance to Cephalosporins and Carbapenems in Penicillin-Allergic Patients. J Investig Allergol Clin Immunol. 2020;30(1):75-76. doi: 10.18176/jiaci.0463. Epub 2019 Nov 4. PMID: 31680067.
- Romano A, Valluzzi RL, Caruso C, Maggioletti M, Quaratino D, Gaeta F. Cross-Reactivity and Tolerability of Cephalosporins in Patients with IgE-Mediated Hypersensitivity to Penicillins. J Allergy Clin Immunol Pract. 2018 Sep-Oct;6(5):1662-1672. doi: 10.1016/j.jaip.2018.01.020. Epub 2018 Feb 3. PMID: 29408440.
Level Up Your Practice
Ready to advance your pharmacy career?
Join thousands of pharmacy professionals learning with PACU.